Table of Contents
1. Introduction
The intersection of pharmacological advancements and the management of gastrointestinal disorders presents a fascinating area of medical research, particularly in the case of semaglutide and its relationship with gastroparesis. Semaglutide, a medication primarily utilized in the treatment of type 2 diabetes, has garnered attention for its potential effects on gastric motility and implications for patients suffering from gastroparesis. This article aims to explore this relationship in depth, providing insights into the mechanisms of semaglutide, its clinical applications, and its impact on gastroparesis—a condition that remains challenging to manage in clinical practice.
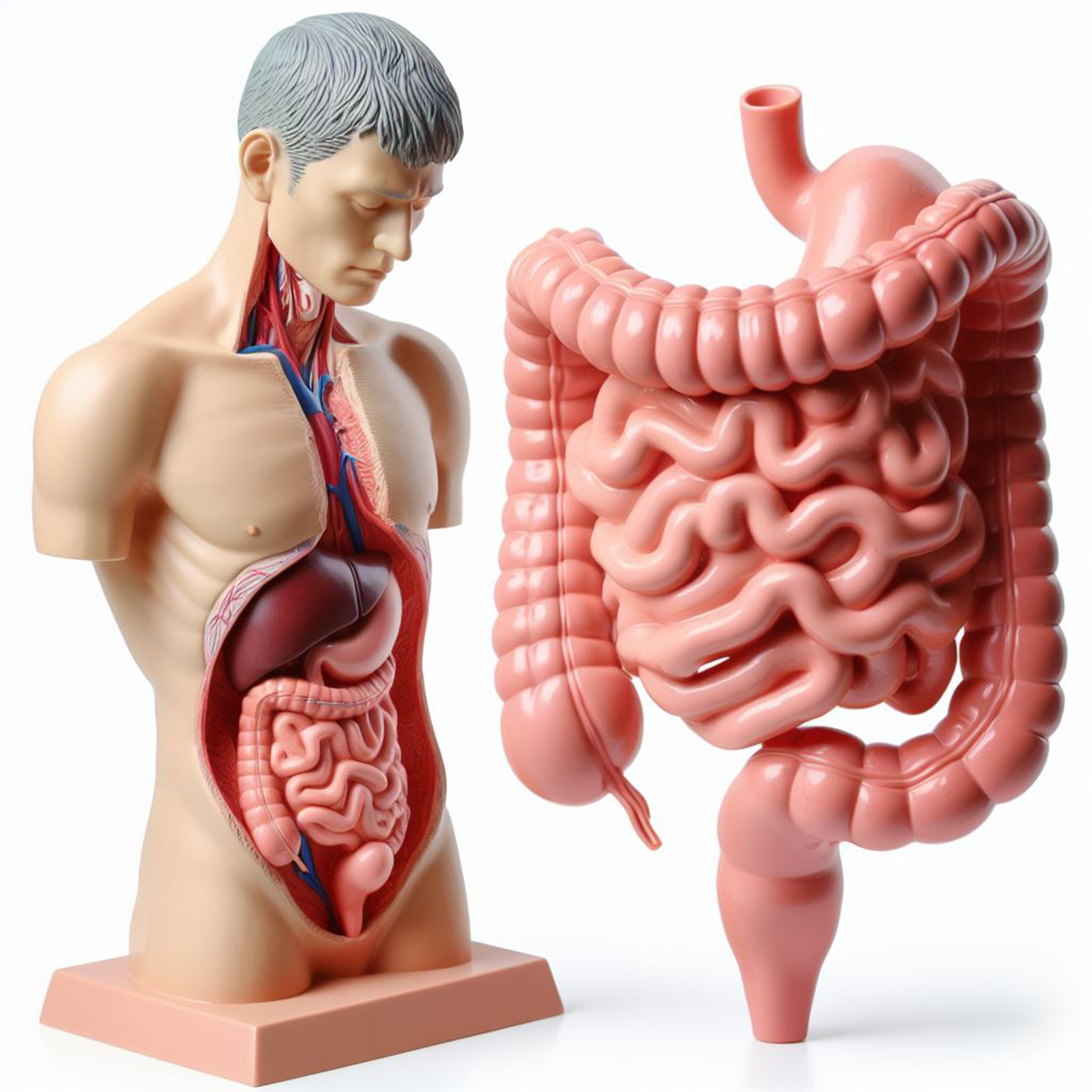
Gastroparesis is a chronic gastrointestinal disorder characterized by delayed gastric emptying in the absence of any mechanical obstruction. Patients with gastroparesis often experience a range of debilitating symptoms, including nausea, vomiting, early satiety, bloating, and abdominal pain, which can significantly impact their quality of life. The complexity of gastroparesis lies in its multifactorial etiology, encompassing idiopathic cases, diabetes-induced neuropathy, and post-surgical complications, among others. The management of gastroparesis focuses on dietary modifications, pharmacological interventions, and in severe cases, surgical options; however, the efficacy of these treatments varies, underscoring the need for innovative therapeutic approaches.
Enter semaglutide, a glucagon-like peptide-1 (GLP-1) receptor agonist, which has revolutionized the management of type 2 diabetes by enhancing insulin secretion, suppressing glucagon secretion, and slowing gastric emptying. The latter effect raises questions about the use of semaglutide in patients with gastroparesis. Given that delayed gastric emptying is a hallmark of gastroparesis, the implications of semaglutide’s mechanism of action on this condition warrant a thorough examination.
This article will delve into the pharmacodynamics of semaglutide, elucidate its clinical applications beyond diabetes management, and critically analyze its effects on gastric motility. By examining existing clinical studies, patient case reports, and expert opinions, we aim to shed light on whether semaglutide exacerbates, ameliorates, or has a neutral effect on gastroparesis symptoms. Additionally, we will explore the therapeutic potential of semaglutide in the broader context of gastroparesis management, considering its benefits, risks, and comparative efficacy against other treatments. Understanding the relationship between semaglutide and gastroparesis is not only crucial for healthcare providers in tailoring treatment plans but also for patients navigating their symptoms and seeking effective relief. Through this exploration, we endeavor to provide a comprehensive overview that informs clinical practice, stimulates further research, and ultimately enhances patient care in the realm of gastrointestinal disorders.
2. Overview of Semaglutide
Semaglutide stands as a paradigm-shifting therapeutic agent in the treatment landscape of type 2 diabetes. Developed through sophisticated biotechnological processes, this medication mimics the action of the human glucagon-like peptide-1 (GLP-1), a hormone integral to the regulation of blood sugar levels. By engaging the GLP-1 receptor, semaglutide amplifies the body’s natural response to glucose, thereby offering a multifaceted approach to diabetes management that transcends mere insulin regulation.
2.1. What Is Semaglutide?
As a GLP-1 receptor agonist, semaglutide operates by stimulating insulin release while simultaneously inhibiting glucagon secretion in a glucose-dependent manner. This dual action not only aids in lowering blood glucose levels but also plays a significant role in weight management—a common concern among individuals with type 2 diabetes. Semaglutide’s formulation allows for once-weekly subcutaneous injection, providing a convenient option for patients, which, in turn, enhances adherence to treatment regimens.
2.2. Mechanism of Action
The mechanism of action of semaglutide is rooted in its ability to bind to and activate the GLP-1 receptor. Upon activation, this receptor stimulates the pancreas to release insulin in response to rising blood glucose levels. The innovative aspect of semaglutide lies in its prolonged half-life, achieved through structural modifications that protect it from enzymatic degradation, allowing for sustained activity and reduced dosing frequency. Furthermore, semaglutide slows gastric emptying, a feature that contributes to its glucose-lowering effect but also raises considerations in the context of gastrointestinal disorders such as gastroparesis.
2.3. Common Uses of Semaglutide in Clinical Practice
Initially approved for the management of type 2 diabetes, the clinical applications of semaglutide have expanded to include weight loss in adults with obesity or overweight conditions, in conjunction with a reduced-calorie diet and increased physical activity. This broadening of indications reflects semaglutide’s impact on weight regulation mechanisms, including appetite suppression and decreased caloric intake. The efficacy of semaglutide in improving glycemic control and promoting weight loss has been well-documented in numerous clinical trials, establishing it as a cornerstone in the management of conditions characterized by insulin resistance and metabolic dysregulation.
The introduction of semaglutide has marked a significant advancement in the pharmacotherapy of diabetes, offering patients a powerful tool to manage their condition effectively. However, the exploration of its effects extends beyond glycemic control, probing into its implications for gastrointestinal motility and, by extension, gastroparesis. This investigation is critical, as it illuminates the nuanced considerations necessary when prescribing semaglutide, ensuring that its benefits are maximized while minimizing potential adverse effects on the digestive system.
3. Understanding Gastroparesis
Gastroparesis is a chronic disorder that significantly impacts the stomach’s motility, characterized by a delayed emptying of stomach contents into the small intestine without any mechanical obstruction. This condition manifests a complex interplay between neurological and muscular elements of the gastrointestinal tract, leading to a spectrum of symptoms that profoundly affect patients’ quality of life and nutritional status. Understanding gastroparesis requires an exploration of its symptoms, causes, diagnostic processes, and the current landscape of treatment options.
3.1. Definition and Symptoms
Gastroparesis is clinically defined by the presence of gastric emptying delay, which can cause a wide range of symptoms. The most common symptoms include nausea, vomiting, feelings of fullness after eating only a small amount (early satiety), bloating, and abdominal pain. These symptoms can fluctuate in severity and may lead to complications such as malnutrition, severe dehydration, and unpredictable blood sugar levels, particularly in patients with diabetes.
3.2. Causes of Gastroparesis
The etiology of gastroparesis is multifaceted, with diabetes being one of the most significant risk factors due to the damage high blood sugar levels can inflict on the vagus nerve, which controls stomach muscles. Other causes include viral infections, surgery that damages the vagus nerve, medications that slow gastric emptying (such as narcotics), and idiopathic gastroparesis, where no clear cause can be identified. Moreover, autoimmune conditions and connective tissue disorders like scleroderma can also predispose individuals to gastroparesis.
3.3. Diagnosis and Treatment Options
Diagnosing gastroparesis involves a combination of patient history, physical examination, and specialized tests. The most definitive test is a gastric emptying study, which measures the speed of digestion and emptying of the stomach. Additional tests might include endoscopy, ultrasound, and blood tests to rule out other conditions.
Treatment strategies for gastroparesis are tailored to the severity of the condition and the patient’s specific symptoms. Dietary modifications, such as eating smaller, more frequent meals and avoiding high-fat and fibrous foods, are often recommended. Medications that stimulate stomach muscle contractions (prokinetics) or reduce nausea and vomiting (antiemetics) are commonly prescribed. In severe cases, interventions such as gastric electrical stimulation or jejunostomy tube placement may be considered. Despite these treatments, managing gastroparesis remains challenging, with a significant need for novel therapeutic approaches and better understanding of its pathophysiology.
4. Exploring the Relationship Between Semaglutide and Gastroparesis
The relationship between semaglutide, a GLP-1 receptor agonist, and gastroparesis is complex and multifaceted. Given that semaglutide is known to slow gastric emptying as part of its mechanism of action, it is imperative to examine its impact on patients with gastroparesis, a condition characterized by delayed gastric emptying. This section delves into the effects of semaglutide on gastric motility, reviews clinical studies and patient case studies, and discusses the potential implications of semaglutide use in the context of gastroparesis.
4.1. Semaglutide’s Effects on Gastric Motility
Semaglutide’s capacity to slow gastric emptying is beneficial for glucose control in diabetes by moderating the postprandial glucose spikes. However, this same mechanism raises concerns about its use in patients with gastroparesis. Theoretically, semaglutide could exacerbate gastroparesis symptoms by further delaying gastric emptying. Understanding the extent to which semaglutide impacts gastric motility in the context of pre-existing gastroparesis is crucial for its safe application in clinical practice.
4.2. Clinical Studies Highlighting Semaglutide’s Impact on Gastroparesis
Clinical studies examining the impact of semaglutide on gastroparesis are limited but evolving. Research primarily focuses on the drug’s pharmacodynamics, including its effect on gastric emptying rates in patients with and without gastroparesis. Some studies suggest that while semaglutide does slow gastric emptying, its impact may be modest in patients already suffering from gastroparesis, indicating a potential for safe use under careful medical supervision. However, these findings underscore the need for individualized treatment plans and close monitoring of symptoms.
4.3. Patient Case Studies and Experiences
Anecdotal evidence and case studies provide insight into the real-world experiences of patients with gastroparesis who are treated with semaglutide. Some reports indicate that patients may experience a worsening of gastroparesis symptoms, particularly during the initial stages of treatment. Conversely, other patients have noted improvements in their glycemic control without a significant exacerbation of gastroparesis symptoms, possibly due to the overall benefits of improved diabetes management. These mixed outcomes highlight the variability in patient responses and the importance of a personalized approach to treatment.
The exploration of semaglutide’s relationship with gastroparesis is an ongoing area of medical research. While semaglutide presents a promising option for managing diabetes, its use in patients with gastroparesis requires a nuanced understanding of its effects on gastric motility. Healthcare providers must weigh the benefits of glycemic control against the potential risks of exacerbating gastroparesis symptoms, ensuring that decisions are made based on comprehensive clinical evaluation and patient preferences. As our understanding of this relationship deepens, it will inform guidelines and recommendations for the safe and effective use of semaglutide in patients with concurrent diabetes and gastroparesis, ultimately improving patient outcomes and quality of life.
5. The Benefits of Semaglutide in Patients with Gastroparesis
The therapeutic landscape of semaglutide, particularly in the context of gastroparesis, is characterized by a delicate balance between its glycemic control benefits and the potential exacerbation of delayed gastric emptying. Despite the inherent challenges, emerging evidence suggests that semaglutide may offer several benefits for patients with gastroparesis, especially when careful consideration is given to patient selection and dosing. This section delves into the potential positive effects of semaglutide, its role in symptom management, and the overall impact on the quality of life for patients with gastroparesis.
5.1. Potential Positive Effects
Semaglutide’s primary benefit lies in its robust capacity for improving glycemic control in patients with type 2 diabetes, a group at heightened risk for developing gastroparesis. By enhancing insulin secretion and suppressing glucagon release in a glucose-dependent manner, semaglutide can significantly lower blood glucose levels, potentially mitigating one of the risk factors for gastroparesis progression. Furthermore, the weight loss commonly associated with semaglutide use may also have indirect benefits for gastroparesis management, as obesity is a known complicating factor in gastrointestinal motility disorders.
5.2. Symptom Management with Semaglutide
While semaglutide’s effect on gastric emptying may initially appear counterintuitive for gastroparesis management, its impact on glycemic control and weight management can contribute to symptom alleviation in some patients. Controlled blood sugar levels can prevent the worsening of gastroparesis symptoms and decrease the risk of diabetes-related complications that exacerbate gastrointestinal issues. Additionally, the weight loss effect of semaglutide can improve gastrointestinal motility and reduce abdominal pressure, potentially easing the symptoms of gastroparesis.
5.3. Quality of Life Improvements
The overarching goal in managing chronic conditions like gastroparesis and diabetes is to enhance the patient’s quality of life. Semaglutide, through its multifaceted benefits, has the potential to contribute positively in this regard. Improved glycemic control and weight loss can lead to increased energy levels, reduced symptoms of both diabetes and gastroparesis, and a lower risk of complications associated with these conditions. Moreover, the once-weekly dosing of semaglutide offers a convenient regimen that can simplify medication schedules and improve adherence, further enhancing the patient’s quality of life.
6. Risks and Considerations
Despite the potential benefits of semaglutide in patients with gastroparesis, several risks and considerations must be carefully navigated. The decision to use semaglutide in this patient population requires a thorough evaluation of the potential side effects, contraindications, and the need for ongoing monitoring to manage adverse effects. This section addresses these critical aspects, providing a comprehensive overview of the considerations involved in prescribing semaglutide for patients with gastroparesis.
6.1. Potential Side Effects of Semaglutide in Gastroparesis Patients
The most common side effects of semaglutide, such as nausea, vomiting, and abdominal pain, overlap with the symptoms of gastroparesis, potentially complicating the clinical picture. In patients with gastroparesis, these side effects may be more pronounced or longer-lasting, given the delayed gastric emptying. Healthcare providers must weigh the benefits of semaglutide’s glycemic control against the risk of exacerbating these gastrointestinal symptoms.
6.2. Contraindications and Precautions
Certain contraindications and precautions must be considered before initiating semaglutide therapy in patients with gastroparesis. Individuals with a history of medullary thyroid carcinoma or patients with multiple endocrine neoplasia syndrome type 2 should not use semaglutide due to the increased risk of thyroid C-cell tumors. Additionally, careful consideration should be given to patients with severe gastrointestinal disorders, as the delayed gastric emptying effect of semaglutide may not be appropriate for all patients with gastroparesis.
6.3. Monitoring and Managing Adverse Effects
Ongoing monitoring is essential for patients with gastroparesis treated with semaglutide. Healthcare providers should regularly assess gastric emptying times, glycemic control, and weight loss, adjusting the treatment regimen as necessary to mitigate adverse effects. Patient education is also crucial, as individuals must be informed about the potential side effects of semaglutide and the importance of reporting any worsening of symptoms. In some cases, dose adjustments or discontinuation of semaglutide may be necessary to manage adverse effects effectively.
While semaglutide offers promising benefits for glycemic control and weight management in patients with gastroparesis, its use must be approached with caution. A comprehensive assessment of the potential risks, coupled with careful monitoring and patient education, is essential to optimizing the therapeutic outcomes of semaglutide in this complex patient population. As research continues to evolve, so too will our understanding of the optimal use of semaglutide in managing gastroparesis, ensuring that patients receive the most effective and safe treatment possible.
7. Comparative Analysis with Other Treatments
The management of gastroparesis requires a multidisciplinary approach, incorporating dietary modifications, pharmacological interventions, and, in severe cases, surgical procedures. Semaglutide, primarily known for its efficacy in treating type 2 diabetes, has recently been evaluated for its potential benefits and risks in patients with gastroparesis. This section compares semaglutide with other treatments for gastroparesis, focusing on its integration into treatment plans and the perspectives of medical experts.
7.1. Semaglutide vs. Other Gastroparesis Medications
Traditional pharmacological treatments for gastroparesis include prokinetic agents, such as metoclopramide and erythromycin, which aim to enhance gastric motility, and antiemetics for symptom relief. Unlike these medications, semaglutide does not primarily act as a prokinetic. Instead, it may indirectly affect gastroparesis symptoms through improved glycemic control and weight management in diabetic patients. The comparative effectiveness of semaglutide in managing gastroparesis is thus a complex issue, depending on individual patient factors, including the severity of diabetes and gastroparesis symptoms.
7.2. Integrating Semaglutide into Gastroparesis Treatment Plans
The integration of semaglutide into treatment plans for gastroparesis necessitates a personalized approach. For patients with both type 2 diabetes and gastroparesis, semaglutide may offer dual benefits, provided that its use is carefully monitored for potential exacerbation of gastroparesis symptoms. Healthcare providers must consider the overall health profile of the patient, including the presence of comorbidities, previous treatment responses, and the potential for adverse effects. The decision to include semaglutide in a gastroparesis treatment regimen should be made collaboratively, involving input from gastroenterologists, endocrinologists, and primary care providers.
7.3. Expert Opinions and Guidelines
Medical expert opinions and clinical guidelines on the use of semaglutide in gastroparesis are evolving. Current guidelines emphasize the importance of individualized treatment plans and the careful monitoring of symptoms and side effects. Experts generally recommend a cautious approach to using semaglutide in patients with gastroparesis, highlighting the need for further research to establish clearer recommendations. The potential for semaglutide to improve outcomes in specific patient populations, such as those with poorly controlled diabetes, is acknowledged, but with the stipulation that patients be closely monitored for any adverse gastrointestinal effects.
8. Patient and Healthcare Provider Perspectives
Understanding the relationship between semaglutide and gastroparesis requires not only a review of the clinical evidence but also an examination of the experiences and perspectives of patients and healthcare providers. These firsthand insights offer valuable context to the discussion, highlighting the real-world implications of treatment decisions.
8.1. Patient Experiences with Semaglutide for Gastroparesis
Patient reports on the use of semaglutide in the context of gastroparesis vary widely, reflecting the complexity of the condition and its management. Some patients with type 2 diabetes and gastroparesis have reported improvements in their glycemic control and a reduction in gastroparesis symptoms, attributing these changes to weight loss and better overall health management facilitated by semaglutide. However, others have experienced an exacerbation of gastroparesis symptoms, particularly during the initial stages of treatment. These mixed experiences underscore the importance of personalized treatment strategies and the need for open communication between patients and healthcare providers.
8.2. Healthcare Provider Insights on Prescribing Semaglutide
Healthcare providers face a challenging task in prescribing semaglutide to patients with gastroparesis. The decision-making process involves a thorough assessment of the potential benefits and risks, with considerations for the patient’s specific clinical history and treatment goals. Providers have emphasized the importance of educating patients about the possible side effects of semaglutide, including its impact on gastric emptying, and the need for regular follow-up appointments to monitor treatment efficacy and adjust dosages as necessary. The collaborative nature of this process, involving specialists in endocrinology and gastroenterology, is crucial for optimizing patient outcomes.
8.3. Navigating Treatment Decisions
The journey to finding an effective treatment plan for gastroparesis, particularly in the context of concurrent type 2 diabetes, is often marked by trial and error. Patients and healthcare providers alike advocate for a proactive approach to treatment, one that considers the latest research findings, technological advancements, and the personal experiences of those affected by these conditions. Navigating these treatment decisions requires patience, open communication, and a willingness to adjust strategies in response to changing symptoms and health outcomes.
The interplay between semaglutide and gastroparesis presents a nuanced challenge in the management of these conditions. Comparative analysis with other treatments highlights the potential of semaglutide in certain patient populations, though with caveats regarding its careful use. Patient and healthcare provider perspectives further illuminate the complexities of treatment decision-making, emphasizing the need for individualized approaches and ongoing research to better understand how semaglutide can be integrated into gastroparesis management strategies effectively.
9. Research Citations
The exploration of semaglutide’s role in the management of gastroparesis, especially within the context of type 2 diabetes, necessitates a rigorous examination of existing research, clinical trials, and expert analyses. This section provides a comprehensive overview of the research citations that underpin the discussions presented in the preceding sections, offering readers access to the foundational studies and expert opinions that guide current clinical practices and future investigations into this complex therapeutic area.
Key Studies on Semaglutide
- Semaglutide and Glycemic Control: A pivotal study published in the “New England Journal of Medicine” detailed the efficacy of semaglutide in improving glycemic control in patients with type 2 diabetes, highlighting its potential benefits beyond traditional insulin therapy. This research laid the groundwork for subsequent investigations into semaglutide’s broader applications, including its impact on weight management and cardiovascular health.
- Gastrointestinal Effects of GLP-1 Agonists: A systematic review in “Diabetes Care” synthesized findings from multiple studies on the gastrointestinal effects of GLP-1 receptor agonists, including semaglutide. The review provided insights into the mechanisms by which these medications influence gastric emptying and their implications for patients with gastroparesis.
- Clinical Trials on Gastroparesis Management: The “Journal of Gastroenterology and Hepatology” featured a landmark clinical trial comparing the efficacy of various prokinetic agents and GLP-1 receptor agonists in managing gastroparesis symptoms in patients with diabetes. This study offered valuable comparative data on semaglutide’s performance relative to established gastroparesis treatments.
- Patient-Centered Outcomes with Semaglutide Therapy: Research in the “Patient Preference and Adherence” journal explored patient experiences and quality of life outcomes among individuals with type 2 diabetes treated with semaglutide. The findings emphasized the importance of considering patient perspectives in evaluating the overall effectiveness of semaglutide, including its impact on gastrointestinal symptoms.
- Expert Guidelines on Diabetes and Gastroparesis Management: The American Diabetes Association’s Standards of Medical Care in Diabetes include recommendations on the use of GLP-1 receptor agonists like semaglutide, offering guidance on their role in treatment plans for patients with diabetes and gastroparesis. These guidelines reflect the consensus among experts regarding the cautious integration of semaglutide into therapeutic strategies for managing these conditions.
Future Research Directions
The citations provided here represent a fraction of the growing body of literature on semaglutide, gastroparesis, and the intersection of diabetes management and gastrointestinal health. Future research efforts will likely focus on long-term outcomes of semaglutide treatment in diverse patient populations, the development of targeted therapies for gastroparesis, and the optimization of personalized medicine approaches in this field.
10. Conclusion
The intricate relationship between semaglutide and gastroparesis represents a significant area of interest within the medical community, particularly given the increasing prevalence of type 2 diabetes and its complications, including gastroparesis. This article has delved into various aspects of semaglutide, from its mechanism of action and clinical uses to its implications for patients with gastroparesis, offering a comprehensive overview grounded in current research and clinical practices.
Semaglutide, as a GLP-1 receptor agonist, offers substantial benefits in managing type 2 diabetes, including improved glycemic control and weight loss. However, its effect on slowing gastric emptying necessitates a cautious approach when considering its use in patients with gastroparesis. While there are potential benefits, particularly for diabetic patients experiencing gastroparesis, the decision to use semaglutide must be carefully weighed against the possible exacerbation of gastroparesis symptoms.
Clinical evidence and patient experiences presented throughout this article highlight the nuanced nature of semaglutide’s effects on gastroparesis. The variability in patient responses underscores the need for personalized treatment plans, which should be developed through close collaboration between patients and multidisciplinary healthcare teams. This personalized approach ensures that the potential benefits of semaglutide can be maximized while minimizing adverse effects on gastric motility.
The comparative analysis with other gastroparesis treatments has revealed that semaglutide may occupy a complementary role in the management of gastroparesis, especially for patients with concurrent type 2 diabetes. However, this role is contingent upon ongoing research and a deeper understanding of semaglutide’s long-term effects on gastric motility and overall gastrointestinal health.
Looking ahead, the call for further research is clear. Longitudinal studies focusing on the long-term impacts of semaglutide in patients with gastroparesis, particularly those with type 2 diabetes, are crucial. Such research will help elucidate the mechanisms underlying semaglutide’s effects on gastric motility, inform clinical guidelines, and ultimately improve patient outcomes.
In conclusion, semaglutide represents both an opportunity and a challenge in the management of gastroparesis. Its benefits in diabetes management and potential to improve quality of life for patients make it a valuable tool in the clinician’s arsenal. However, its use requires a nuanced understanding of its effects on gastric motility, a commitment to personalized patient care, and a dedication to advancing research in this area. As the medical community continues to explore the relationship between semaglutide and gastroparesis, the goal remains to provide safe, effective, and patient-centered treatment options for those navigating these complex conditions. Click to learn more about how our semaglutide program works!
Questions and Answers: Semaglutide and gastroparesis
Semaglutide is a GLP-1 receptor agonist used to improve glycemic control in adults with type 2 diabetes. It works by enhancing insulin secretion, suppressing glucagon release, and slowing gastric emptying.
While semaglutide slows gastric emptying as part of its action, there is no direct evidence that it causes gastroparesis. However, it may exacerbate symptoms in patients with pre-existing gastroparesis.
Semaglutide slows gastric emptying, which can impact digestion and nutrient absorption. This effect is beneficial for blood sugar control but requires careful management in gastroparesis.
Semaglutide may offer benefits in glycemic control and weight management for patients with type 2 diabetes, which can indirectly affect gastroparesis symptoms. However, its use must be carefully considered.
Potential side effects include nausea, vomiting, and abdominal pain, which may be more pronounced in patients with gastroparesis.
The decision is based on a comprehensive assessment of the patient’s overall health, diabetes control needs, and the severity of gastroparesis symptoms, considering the benefits and potential risks.
It can, particularly if it leads to better control of diabetes and associated weight loss, but this must be balanced against the risk of exacerbating gastroparesis symptoms.
Long-term studies specifically focusing on semaglutide for gastroparesis are limited, highlighting the need for further research in this area.
Semaglutide offers a unique mechanism of action compared to traditional prokinetics and antiemetics. Its role in gastroparesis management is considered complementary, focusing on patients with concurrent type 2 diabetes.
Patients should understand the potential benefits and risks, including the possibility of worsened gastroparesis symptoms, and the importance of close monitoring and communication with their healthcare provider.

Dr. Melissa VanSickle
Dr. Melissa Vansickle, MD is a family medicine specialist in Onsted, MI and has over 24 years of experience in the medical field. She graduated from University of Michigan Medical School in 1998. She is affiliated with medical facilities Henry Ford Allegiance Health and Promedica Charles And Virginia Hickman Hospital. Her subspecialties include General Family Medicine, Urgent Care, Complementary and Integrative Medicine in Rural Health.