Table of Contents
Introduction
Tirzepatide is a medication that helps people manage blood sugar and lose weight. It works by copying the effects of two natural hormones in the body—GIP and GLP-1. These hormones help the body use insulin better, slow down digestion, and reduce hunger. Because of how it works, tirzepatide is used to treat adults with type 2 diabetes and is also approved to help people who are overweight or have obesity lose weight. It is given as a shot under the skin, usually once a week.
This medication is sold under the brand name Mounjaro® for type 2 diabetes and Zepbound® for weight management. Both are prescription medications. That means a healthcare provider must decide if the medication is safe and right for the person before giving a prescription. Once prescribed, tirzepatide can be picked up at a pharmacy or sometimes given at a clinic or doctor’s office.
Since tirzepatide is not sold over the counter, people often want to know where to go to get it. Many wonder if it is only available through specialists like endocrinologists or if it can also be prescribed by a primary care doctor. Others want to know if their insurance will help cover the cost or if they need to pay out of pocket. Questions also come up about how to schedule an appointment, what information is needed, and how to prepare for the first visit.
Access to tirzepatide can feel confusing, especially when insurance rules, provider availability, and pharmacy supply vary by location. There are also limits on who qualifies for the medicine based on their health history, body mass index (BMI), and other conditions. Many people search online to figure out how to start the process, but the information is often scattered or hard to understand.
This article gives a full and easy-to-understand guide on how to get a tirzepatide shot. It answers the most common questions people search for when looking for doctors or clinics that offer tirzepatide. It also explains how to check insurance coverage, what to expect when scheduling an appointment, and how to prepare for follow-up visits. This includes step-by-step help on locating healthcare providers, finding out if tirzepatide is covered by a specific insurance plan, and tips to make the process smoother. Readers will learn who is allowed to prescribe the shot, what types of clinics give it, and whether telehealth visits are an option. There is also information about what happens after the first appointment, including how to refill the medication and when to return to the doctor.
This guide is designed to be helpful for people who are just beginning to explore tirzepatide and for those already in the process of trying to get a prescription. Each section gives medical facts and practical advice to help readers feel more confident about their next steps. While the information is based on current medical and insurance practices in the United States, many parts of the process may also apply in other places.
By the end of this article, readers will have a clear understanding of what tirzepatide is, how to find a doctor or clinic that offers it, what role insurance plays, and what to expect when starting treatment. No opinions or personal stories are included—just the facts and steps needed to get a tirzepatide shot safely and correctly.
What Types of Healthcare Providers Can Administer Tirzepatide?
Tirzepatide is a medication used to treat type 2 diabetes and to help with weight loss in people with obesity. It is given as a weekly injection under the skin. It is sold under the brand name Zepbound® for weight management and Mounjaro® for diabetes treatment. Because it is a prescription drug and is injected, only licensed healthcare professionals are allowed to prescribe it and, in some cases, administer it.
This section explains which types of providers can help patients start tirzepatide and what role each one may play.
Endocrinologists
An endocrinologist is a doctor who specializes in treating hormone-related problems, including diabetes. Endocrinologists are experts in blood sugar control and are highly trained in using medicines like tirzepatide. They can write a prescription and help with starting the injection. They also watch for side effects and make sure the dose is right over time.
Patients who have type 2 diabetes or complicated medical histories are often referred to endocrinologists. These specialists usually practice in hospitals, diabetes clinics, or specialty medical offices. Many patients see them after their primary care doctor recommends it.
Primary Care Providers (PCPs)
Many people get tirzepatide through their primary care provider (PCP). This includes family doctors, internal medicine doctors, and sometimes pediatricians who care for teens with obesity or diabetes. PCPs often help patients with long-term health conditions like obesity, high blood pressure, and diabetes.
Primary care providers can write prescriptions for tirzepatide. They may also teach patients how to give the injections at home. If needed, they can refer patients to other specialists. In some cases, PCPs may want lab tests or documentation before starting the medication.
Obesity Medicine Specialists
Doctors who focus on weight loss and obesity treatment are called obesity medicine specialists. These providers are trained to manage weight-related conditions using a full treatment plan. This may include diet changes, exercise, behavior support, and medications like tirzepatide.
Obesity specialists may be board certified by the American Board of Obesity Medicine (ABOM). They often work in private clinics or medical weight loss centers. These providers are skilled in choosing the right weight loss medication for each patient. They monitor progress and adjust the dose as needed.
Nurse Practitioners (NPs) and Physician Assistants (PAs)
Nurse practitioners (NPs) and physician assistants (PAs) are licensed healthcare professionals who can diagnose, treat, and prescribe medications. In most states in the U.S., NPs and PAs are allowed to prescribe tirzepatide. Their ability to do this may depend on state laws and whether they work under the supervision of a doctor.
NPs and PAs are commonly found in primary care offices, weight loss clinics, and endocrinology practices. They often help with education and patient follow-up. They may also give the first injection in the clinic and teach the patient how to do it at home.
Telehealth Providers
Some licensed doctors, NPs, and PAs offer telehealth services. This means patients meet with them online using a video or phone call. Telehealth providers can evaluate a person’s medical history and, if appropriate, prescribe tirzepatide. However, not all states allow controlled or injectable medications to be prescribed by telehealth. Some insurance plans may also have rules about this.
For patients who live far from a specialist, telehealth may be a helpful option. The prescription is usually sent to a pharmacy, and the patient may give the shot at home or go to a clinic to receive it.
Pharmacists (Administration Only, in Some States)
In a few U.S. states, pharmacists can administer certain injectable medications after a doctor prescribes them. These rules vary by location. Even in states where this is allowed, pharmacists do not diagnose or decide on the medication. They only give the shot if a valid prescription is already in place.
This is more common in large chain pharmacies or clinics inside pharmacies, such as retail health locations. Patients should check with their local pharmacy to see if this service is available for tirzepatide.
Legal and Practice Guidelines
Each U.S. state has laws about who can prescribe and administer injectable medications like tirzepatide. Most of the time, doctors, nurse practitioners, and physician assistants can write the prescription and guide the treatment. In a few states, pharmacists can help with administration. However, each provider must follow their licensing rules and the policies of the clinic or health system where they work.
Tirzepatide is a powerful medication that requires a prescription and close monitoring. Many types of healthcare providers can help patients start treatment, including endocrinologists, primary care doctors, obesity specialists, nurse practitioners, and physician assistants. Telehealth and pharmacy services may also be options in some areas. To begin tirzepatide safely, it is important to work with a qualified provider who understands how the medication works and what to watch for.
Where Can Tirzepatide Injections Be Prescribed or Given?
Tirzepatide is a prescription medicine used to help people manage type 2 diabetes and, in some cases, obesity. It is sold under the brand name Mounjaro®. This medication is given as a shot under the skin once a week. Patients need a licensed medical provider to prescribe tirzepatide. In many cases, the provider also helps with teaching how to use the shot or gives the injection in the clinic.
Finding the right place to get tirzepatide involves knowing what types of clinics or doctors offer it. It also helps to know how to search for them and what tools are available to make this easier.
Types of Clinics That Offer Tirzepatide
Several types of clinics and healthcare centers may offer tirzepatide shots or prescriptions. These include:
- Endocrinology Clinics
Endocrinologists are doctors who treat hormone-related conditions. Many endocrinology clinics help patients with diabetes and weight concerns. These clinics are among the most common places to get tirzepatide prescribed. They are also likely to follow up with patients regularly and adjust doses when needed.
- Primary Care Clinics
Some primary care providers, such as family doctors or internal medicine physicians, may also prescribe tirzepatide. This usually happens if they are already treating a patient for type 2 diabetes or if the clinic has experience with weight loss medications. However, not all general doctors are familiar with newer medications like tirzepatide, so availability may vary.
- Diabetes Management Centers
Specialized diabetes centers often provide a full team of care, including doctors, nurses, and diabetes educators. These centers can prescribe tirzepatide and train patients on how to use the injection properly. They may also offer nutrition and blood sugar monitoring support.
- Weight Management Clinics
Some clinics that focus on medical weight loss use medications like tirzepatide to support treatment plans. These centers usually offer in-depth support such as meal planning, behavior therapy, and tracking weight changes. It is important to make sure the clinic has licensed professionals qualified to prescribe injectable medications.
- Academic Medical Centers or Teaching Hospitals
Large hospitals linked to medical schools often offer new treatments and have specialists on staff. These centers may have research programs or specialty departments using tirzepatide. They may also be involved in clinical trials for similar medications.
How to Find Doctors and Clinics That Offer Tirzepatide
Locating a clinic or provider who offers tirzepatide involves doing a bit of research. Several options can help with this:
- Use Health Insurance Provider Directories
Most insurance companies have online tools to help patients find doctors and clinics covered by their plans. These directories allow users to search for doctors by name, location, and specialty. Typing in “endocrinologist,” “diabetes care,” or “weight management” in the search box may help locate nearby clinics.
- Contact Local Pharmacies
Pharmacists often know which local clinics prescribe certain medications. Some pharmacies may also carry tirzepatide or help with ordering it through specialty channels. Talking to the pharmacist can give clues about which doctors regularly prescribe Mounjaro® in the area.
- Search on the Official Mounjaro® Website
The drug manufacturer often offers a provider locator tool. For Mounjaro®, the official website (www.mounjaro.com) may list clinics and doctors who prescribe the medication. These tools usually ask for a ZIP code and show a list of providers nearby.
- Online Health Platforms and Databases
Websites such as Healthgrades, Zocdoc, or Vitals list doctors by specialty and patient ratings. Some of these platforms let users filter by treatment type, including diabetes medications or weight loss treatments. These services often include appointment availability and reviews.
- Call Local Clinics Directly
Sometimes, the fastest way to find out is by calling nearby clinics or sending a message through their websites. Ask if they prescribe tirzepatide and if they are accepting new patients. Some clinics may require a referral or initial visit before writing a prescription.
Important Notes About Availability
Not every clinic or provider will offer tirzepatide. Some doctors may not be familiar with the medication, or they may only prescribe it for certain medical conditions. In other cases, clinics may not have enough supply or may wait until insurance approval comes through.
It is also important to make sure that the person prescribing the medication is licensed to do so. Only licensed medical professionals—such as medical doctors (MDs), nurse practitioners (NPs), or physician assistants (PAs)—can legally prescribe tirzepatide.
Many different clinics may offer tirzepatide, including endocrinology practices, diabetes centers, and some weight loss programs. The best place to start is often with a patient’s current doctor or health plan provider. Other helpful tools include online directories, pharmacy contacts, and drug manufacturer websites.
Is Tirzepatide Available at Pharmacies or Retail Clinics?
Tirzepatide is a prescription medication used to treat type 2 diabetes and support weight loss in certain adults. It is sold under the brand name Zepbound® for weight management and Mounjaro® for diabetes. Both are injectable medications that must be prescribed by a licensed healthcare provider.
Many people wonder if tirzepatide can be picked up at a pharmacy like a regular medicine or if it must be given in a clinic. This section explains where tirzepatide is available, how it is given, and what role pharmacies and retail clinics play in this process.
Tirzepatide Requires a Prescription
Tirzepatide is not an over-the-counter medicine. It cannot be bought without a prescription. A licensed doctor, nurse practitioner, or physician assistant must evaluate the patient and decide if tirzepatide is safe and appropriate. After the prescription is written, it is usually sent to a pharmacy.
There are two common ways patients receive tirzepatide:
- The doctor gives the injection at the clinic.
- The pharmacy fills the prescription, and the patient gives the injection at home.
Both options depend on the provider’s setup and the patient’s needs.
In-Office Injections vs. Self-Administration
Some healthcare clinics offer in-office injections. In this case, the patient visits the clinic regularly and a nurse or medical assistant gives the shot. This can be helpful for patients who are nervous about injecting themselves or who need support with technique or side effects.
Other times, the healthcare provider may prescribe tirzepatide for self-injection at home. In this case, the patient picks up the medication from the pharmacy. The shot is usually given once a week. Patients are trained on how to use the injection device, which is a single-dose prefilled pen.
This pen is designed to be simple to use, but patients still need to learn how to:
- Store the medication correctly (usually in the refrigerator)
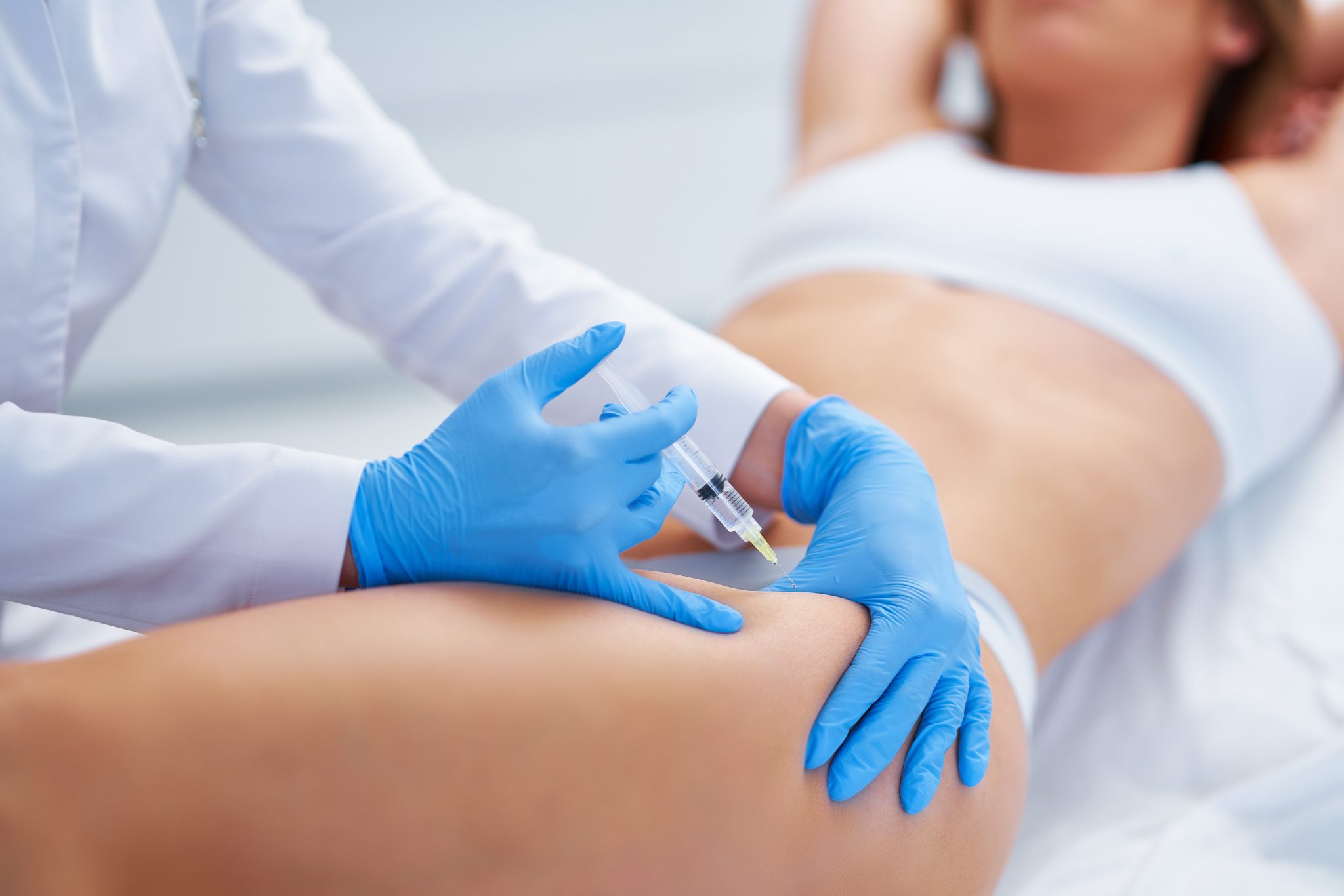
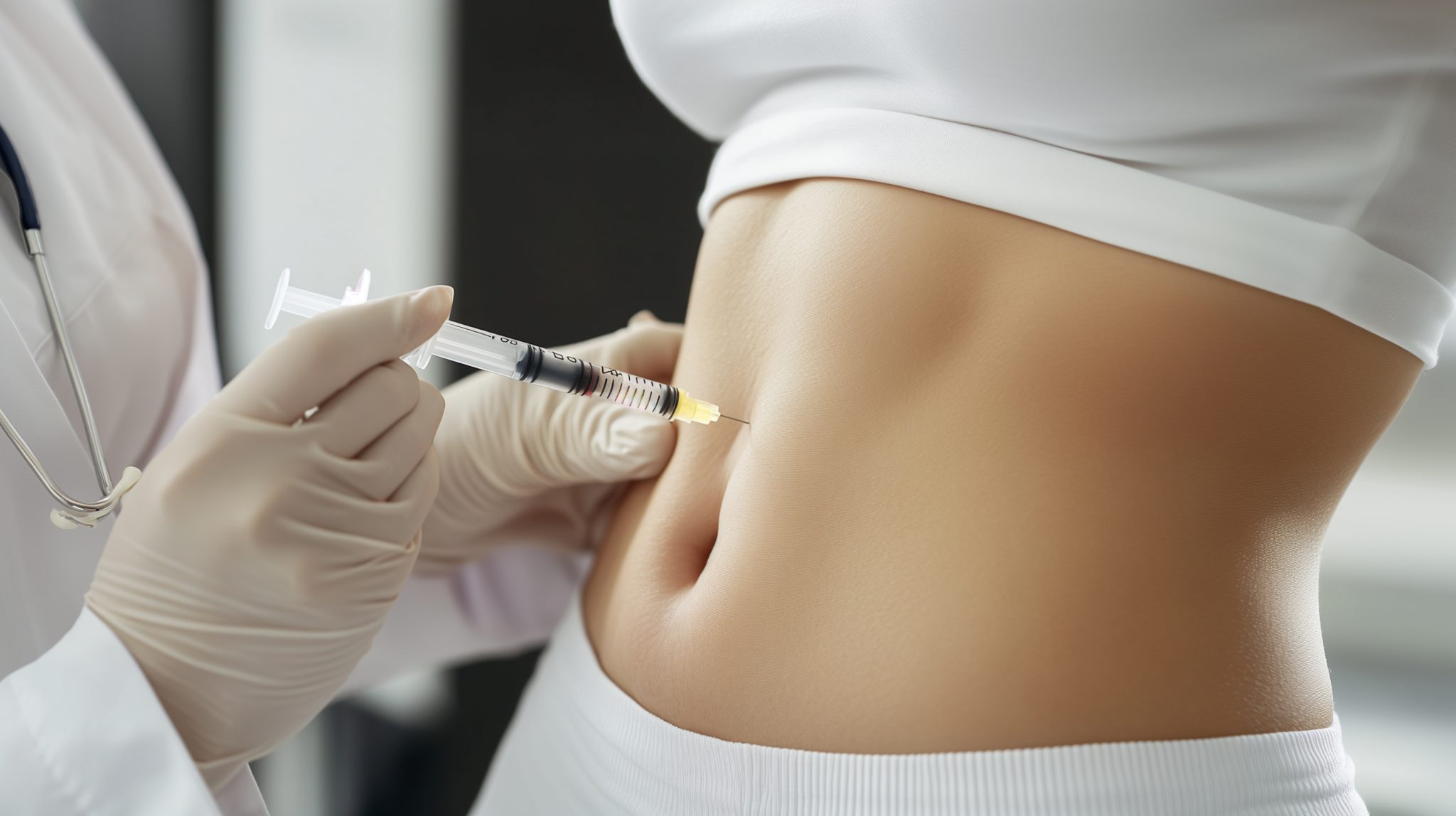
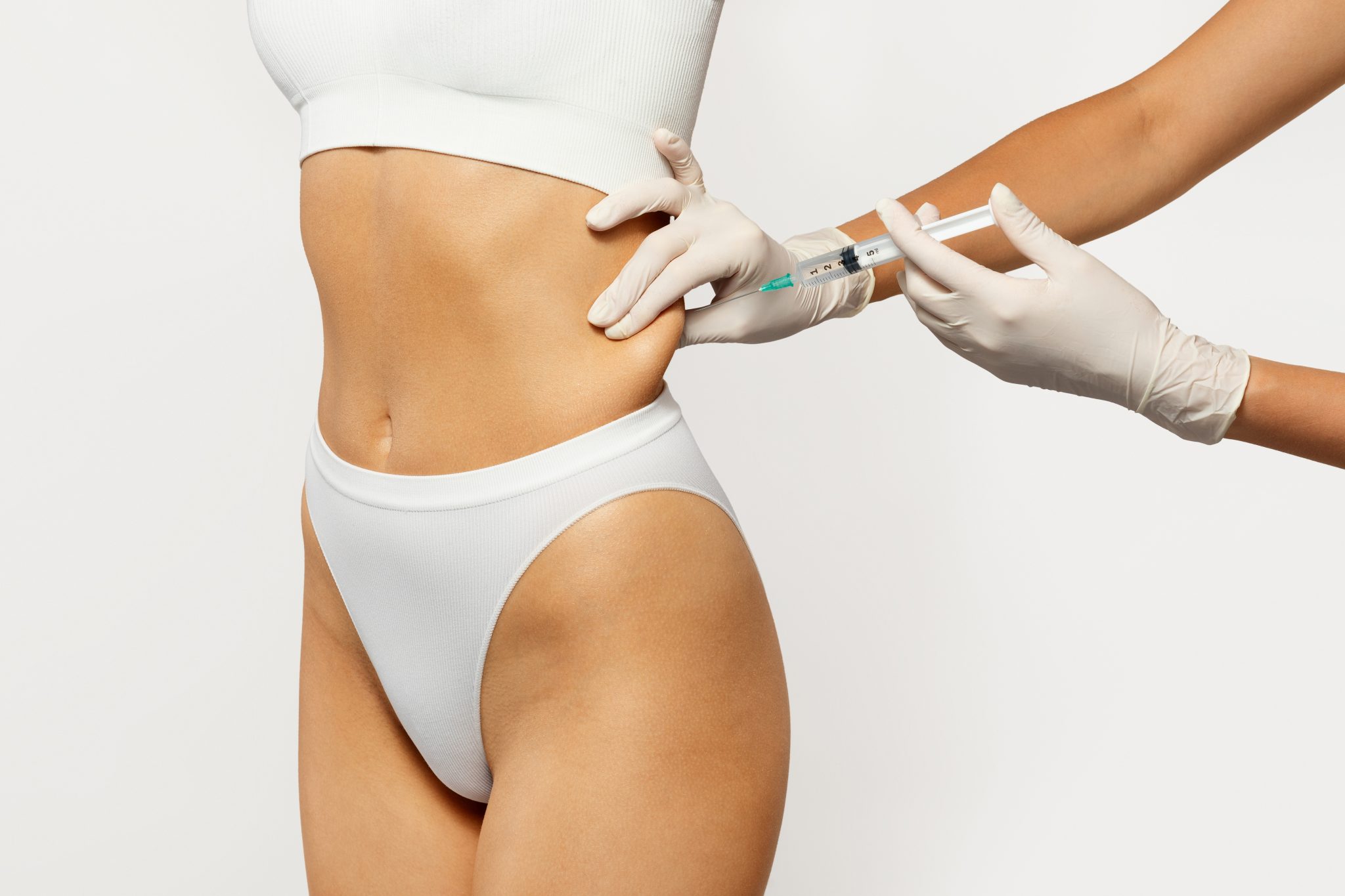
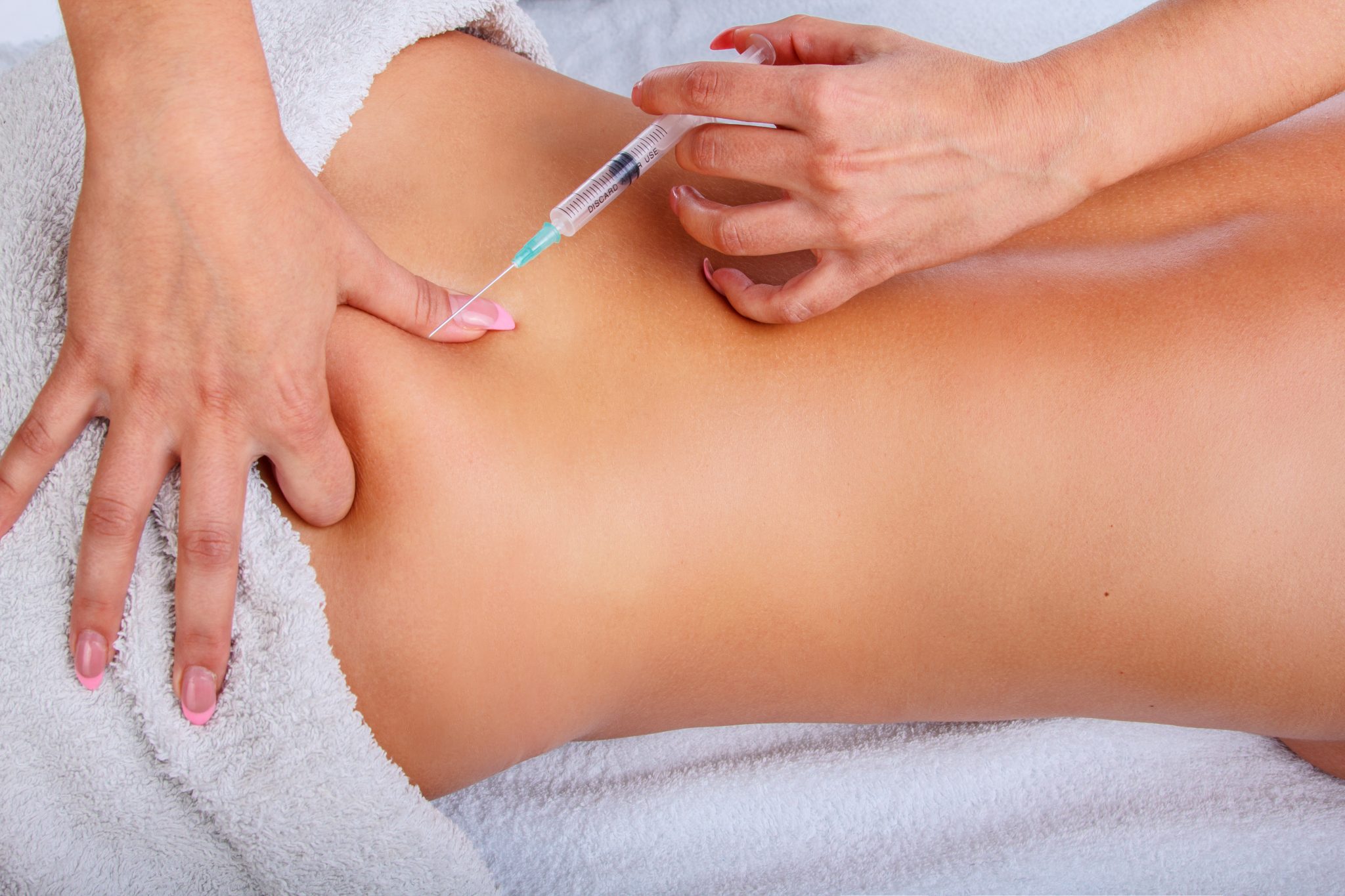
- Choose the right injection site (such as the stomach, thigh, or upper arm)
- Use the pen properly and safely
- Dispose of the used pen correctly
Most providers will give an in-person or video demonstration before the first injection is given at home.
Role of Pharmacies in Accessing Tirzepatide
Many pharmacies can fill tirzepatide prescriptions, but not all stock it. This is because tirzepatide is a specialty drug. It must be stored at certain temperatures, and it can be expensive. Common options include:
- Local retail pharmacies (such as CVS®, Walgreens®, or Walmart®): Some locations may carry tirzepatide, but patients should call ahead to ask if it is in stock.
- Mail-order or specialty pharmacies: Insurance companies often require patients to use a specialty pharmacy. These pharmacies are used to handling expensive medications and often ship the medicine with cold packs to protect it.
The doctor’s office may help with sending the prescription to the correct pharmacy. Some clinics have coordinators who check with the insurance company and confirm which pharmacy to use.
Retail Clinics and Walk-In Options
Retail clinics are health clinics inside stores like CVS®, Walgreens®, or Kroger®. These clinics are staffed by nurse practitioners or physician assistants. They offer care for minor illnesses, health screenings, and some treatments.
Tirzepatide is not usually available at walk-in clinics. These clinics do not usually manage long-term medications like diabetes or weight loss injections. Instead, patients must see a primary care doctor, endocrinologist, or obesity medicine specialist. The specialist evaluates health history, monitors progress, and adjusts the dose as needed.
However, some retail clinics may help with:
- Reviewing injection technique
- Giving follow-up injections (if approved)
- Answering questions about side effects
It is important to call ahead and ask if the clinic offers these services.
Tirzepatide is a prescription injectable drug that is either given in a healthcare provider’s office or prescribed for use at home. Pharmacies can fill the prescription, but because tirzepatide is a specialty drug, not all pharmacies carry it. Some patients may need to use a mail-order pharmacy. Retail clinics usually do not start tirzepatide treatment but may support patients who are already using it.
To get tirzepatide safely and correctly, a patient must first speak with a qualified healthcare provider. The doctor will decide the best way to receive the medication—either in the clinic or through home injection after proper training.
How to Check If Insurance Covers Tirzepatide
Before starting tirzepatide treatment, it is important to check if the medication is covered by insurance. Tirzepatide is a prescription injection used for managing type 2 diabetes and, in some cases, for chronic weight management. The cost of tirzepatide can be high without coverage, so understanding the insurance process can help prevent unexpected expenses.
Step 1: Understand How Tirzepatide Is Billed
Tirzepatide may be billed under one of two categories:
- Pharmacy Benefit: This is the same part of insurance that covers most medications picked up at a pharmacy. When tirzepatide is filled at a pharmacy, it is typically billed through this benefit. Patients may self-inject the medication at home after receiving proper instructions from a healthcare provider.
- Medical Benefit: If tirzepatide is given at a doctor’s office or clinic as an in-office injection, it may be billed as a medical procedure. In this case, the medication and the administration may fall under the medical benefit portion of the health insurance plan.
It is important to know which type of benefit applies because each one may have different requirements, costs, and approval processes.
Step 2: Check the Insurance Plan’s Formulary
A formulary is a list of medications covered by a health insurance plan. Most insurance companies have separate formularies for pharmacy and medical benefits. Checking the formulary helps confirm if tirzepatide is included.
To find the formulary:
- Visit the insurance company’s website.
- Log in to the member portal, if available.
- Look for a section labeled “Covered Drugs,” “Prescription Benefits,” or “Formulary List.”
- Search for tirzepatide or a brand name like Zepbound® or Mounjaro®, depending on the treatment goal (weight management or diabetes).
- If unsure, calling the insurance company’s customer service line is another way to confirm.
If tirzepatide is listed, check the tier level. Medications in higher tiers usually cost more. Many insurance plans place tirzepatide in a specialty or high-cost tier.
Step 3: Understand Prior Authorization Requirements
Even if tirzepatide is on the formulary, many insurance plans require prior authorization. This means the doctor must submit documents to show that the medication is medically necessary. The insurance company will review the request and either approve or deny coverage.
Common details that may be required for prior authorization include:
- A diagnosis of type 2 diabetes or obesity with related health conditions.
- A history of trying other medications, such as metformin or GLP-1 medications.
- Body Mass Index (BMI) that meets treatment guidelines (usually BMI ≥ 30 or ≥ 27 with comorbidities).
- Recent lab results or health records that support the need for treatment.
The doctor’s office often handles this process, but delays may occur if additional paperwork is needed. If the request is denied, there may be an appeal process.
Step 4: Ask About Step Therapy and Quantity Limits
Step therapy means the insurance plan may ask for proof that other medications were tried first. For example, the patient might need to try a GLP-1 medication like semaglutide before moving to tirzepatide. This process must be followed before approval is granted.
Quantity limits are another type of restriction. Insurance plans may limit how much tirzepatide can be filled each month. If a higher dose is needed, extra approval may be required.
Step 5: Call the Insurance Provider for Clarification
To avoid confusion, calling the insurance company’s customer service line can be helpful. The phone number is usually on the back of the insurance card. When calling, it helps to ask:
- Is tirzepatide (Zepbound® or Mounjaro®) covered under my plan?
- Is it under pharmacy or medical benefit?
- What tier is it in?
- Is prior authorization required?
- Are there step therapy or quantity limits?
Having the National Drug Code (NDC) from the prescribing provider or pharmacy may help speed up the process.
Step 6: Explore Manufacturer Support Programs
Some patients may be eligible for savings programs offered by the manufacturer. These co-pay cards or patient assistance programs can lower the cost, especially for those with commercial (non-government) insurance. Manufacturer websites such as Zepbound.com or Mounjaro.com provide program details, eligibility, and application forms.
Patients with Medicare, Medicaid, or other federal insurance programs may not qualify for these savings cards, but they can still contact the manufacturer to ask about alternative support options.
By checking each of these areas—formulary, benefit type, prior authorization, step therapy, and cost assistance—patients and healthcare providers can better plan for treatment and reduce the chance of delays in getting tirzepatide.
What Are the Common Insurance Hurdles for Tirzepatide?
Tirzepatide is a prescription injectable medication approved to help manage type 2 diabetes and assist with weight loss in certain individuals. Brand names like Mounjaro® and Zepbound® are two versions of tirzepatide currently available in the United States. These medications can be expensive, so many people rely on insurance coverage to afford them. However, insurance coverage for tirzepatide is not always simple. Several common hurdles may affect whether a patient can get the medication, how soon it is approved, and how much it will cost out-of-pocket.
High Out-of-Pocket Costs
One of the biggest challenges is the cost-sharing structure set by insurance plans. Even when insurance covers tirzepatide, patients may still have to pay part of the cost. These out-of-pocket costs come in different forms:
- Deductibles: A deductible is the amount a person must pay for healthcare services before the insurance plan starts to pay. If a deductible has not been met for the year, the full price of the medication may be required up front.
- Copayments: Some insurance plans charge a fixed amount, or copay, each time a prescription is filled. For specialty drugs like tirzepatide, the copay may be higher than for regular prescriptions.
- Coinsurance: Instead of a fixed copay, some plans use coinsurance, where the patient pays a percentage of the medication cost. For example, if coinsurance is 30% and the monthly cost of tirzepatide is $1,000, the patient must pay $300 every month.
Tirzepatide is often placed on a high “tier” in a health plan’s formulary (the list of approved medications). Specialty drugs are commonly placed in Tier 3 or Tier 4, which usually comes with higher out-of-pocket costs.
Prior Authorization Requirements
Most insurance companies require prior authorization before they agree to pay for tirzepatide. This means a doctor must send paperwork to the insurance company explaining why the medication is needed. The insurer reviews the request and decides if the medication meets its rules for coverage.
The approval process can take several days or even weeks. Common requirements that insurers look for in a prior authorization request include:
- Diagnosis of type 2 diabetes or obesity (based on BMI criteria).
- Proof that the patient has tried and failed other treatments such as metformin, lifestyle changes, or other GLP-1 medications.
- Clinical justification explaining why tirzepatide is the best option.
If the request is incomplete or the criteria are not met, the insurer may deny the medication. This can delay treatment and require an appeal or resubmission by the healthcare provider.
Step Therapy Protocols
Step therapy is a policy used by many insurers to control costs. Under step therapy, the insurance company may require a patient to try other lower-cost medications first before approving tirzepatide. Only if those treatments fail or cause side effects will tirzepatide be approved.
For example, a patient may need to try a different medication like semaglutide or metformin and prove it was not effective. This process can delay the start of tirzepatide treatment even when a doctor recommends it.
Quantity Limits
Another barrier is quantity limits. Insurance plans often limit how much medication can be dispensed in one fill or over a specific time. This might include:
- Limiting the number of pens per month.
- Requiring a set dosage progression (dose escalation schedule) rather than starting at a higher dose.
These limits are often based on FDA-approved labeling or clinical guidelines. However, they can be frustrating if a patient needs a different dose or refill schedule. The healthcare provider may need to submit additional documentation to request an exception.
Coverage Differences Between Medical and Pharmacy Benefits
Tirzepatide may be covered under either the pharmacy benefit or the medical benefit, depending on how the drug is dispensed and administered. This can lead to confusion.
- If the medication is picked up at a pharmacy and used at home, it usually falls under the pharmacy benefit.
- If the injection is given at a doctor’s office, it may fall under the medical benefit.
Each benefit has its own rules, copays, deductibles, and prior authorization process. Patients and clinics must check which benefit applies to avoid coverage delays or surprise bills.
Getting insurance approval for tirzepatide can involve several challenges. These include high out-of-pocket costs, prior authorization paperwork, step therapy rules, quantity limits, and confusion over benefit types. Each insurance plan has different rules, so it is important for healthcare providers and patients to work closely with insurance companies and pharmacies. Careful planning can help reduce delays and improve access to this important medication.
How Can Patients Prepare for Insurance Pre‑Authorization?
Getting insurance approval for a tirzepatide prescription can take time. Most insurance plans require prior authorization before covering the medication. This means that the doctor or clinic must send paperwork to the insurance company to explain why tirzepatide is needed. Without this approval, the patient may have to pay the full price out of pocket, which can be thousands of dollars each month.
This section explains what information is needed, who helps with the paperwork, and how to follow up with the insurance company.
Why Insurance Pre‑Authorization is Needed
Tirzepatide is a high-cost injectable medication, often used to treat type 2 diabetes and, in some cases, for weight management. Because of the cost and medical use, insurance companies want to make sure it is medically necessary. They often check if the patient meets specific rules, called clinical criteria, before agreeing to pay for the drug.
Documents Often Required by Insurance
To start the pre‑authorization process, the doctor’s office will usually collect and submit several important documents. These include:
- A recent diagnosis of type 2 diabetes or, in some cases, obesity with a related condition such as high blood pressure or sleep apnea.
- Body weight and BMI (Body Mass Index) records. Most insurance plans require a BMI over a certain number (such as 30, or 27 with other health issues).
- Medical history, including which other medications were tried in the past and why they did not work well or were not tolerated.
- Lab results, such as A1C blood test results, may also be needed to show current diabetes control.
- Progress notes or chart documentation from the medical provider.
The doctor’s office usually fills out a special prior authorization form, which is provided by the insurance company or pharmacy benefit manager (PBM).
Who Sends the Paperwork
The provider’s clinic staff is typically responsible for submitting the paperwork. This may be a nurse, medical assistant, or someone in the prior authorization department. They gather the needed documents and send them by fax, secure email, or through an online portal.
Some clinics are experienced and send pre‑authorization requests often. These clinics may complete the process quickly. Other clinics may take longer, especially if they are less familiar with the process for specialty medications like tirzepatide.
Timelines for Pre‑Authorization
After the paperwork is sent, insurance companies usually respond within 3 to 10 business days, depending on the plan. If the request is approved, the clinic or pharmacy will be notified. If the request is denied, there is a process to file an appeal or send more documents.
It is important to know that the process may need follow-up. If information is missing, the insurance company may delay or deny the request. Sometimes, they ask for extra details, such as doctor’s notes or new test results.
Tips to Help Speed Up the Process
To make the process smoother, certain steps can help:
- Keep personal health records updated. This includes recent weight, A1C levels, and a list of medications used in the past.
- Make sure the provider’s office has the correct insurance details, including the insurance ID number, plan name, and group number.
- Ask if the clinic uses a specialty pharmacy that helps with pre‑authorization. These pharmacies often offer support teams who work with both clinics and insurance plans.
- Check for manufacturer support. The maker of tirzepatide (such as Mounjaro®) may offer patient assistance programs, co-pay cards, or help with insurance navigation. These programs sometimes include nurse or pharmacist support for paperwork.
- Follow up with the clinic after a few days to confirm that the paperwork was submitted and ask if any updates were received.
What Happens After Approval
Once insurance approval is received, the clinic or pharmacy will contact the patient. They will explain how to pick up the prescription or how it will be shipped. Some insurance plans only allow the drug to be dispensed through a specialty pharmacy. These pharmacies may call to schedule delivery and offer injection training or support.
If the request is denied, the provider can send an appeal letter. This may include more medical history or a detailed explanation from the doctor.
Preparing for insurance pre‑authorization is an important step in getting tirzepatide. Success depends on careful documentation, clinic support, and insurance rules. Patients who understand the process and stay informed can reduce delays and increase the chances of receiving coverage for this medication.
What Should Be Expected When Booking an Appointment?
Booking an appointment for a tirzepatide injection may feel overwhelming at first. However, understanding the steps involved can help make the process smoother. This section explains what patients should expect when contacting a clinic, how to communicate clearly with the staff, and how to prepare before the appointment is confirmed.
Understanding the Purpose of the Appointment
Tirzepatide is a prescription injectable medication. It is often used for managing type 2 diabetes or for chronic weight management, depending on how it is prescribed. Before receiving a shot, a healthcare provider must first evaluate whether the medication is right for the individual’s condition.
The first appointment is usually a consultation. During this visit, the provider reviews the patient’s medical history, current medications, and any weight or blood sugar issues. Only after this step is completed can the provider determine if tirzepatide (sold under the brand name Zepbound® for weight loss or Mounjaro® for diabetes) is appropriate.
Calling or Messaging a Clinic: What to Say
Before making an appointment, it helps to contact the clinic to confirm whether they offer tirzepatide treatment. Not all doctors prescribe this medication. When calling, it is important to be clear and specific. Patients may ask the clinic staff questions like:
- “Does your office currently prescribe tirzepatide?”
- “Is there a provider here who manages weight loss or diabetes treatment using medications like Mounjaro® or Zepbound®?”
- “Are you accepting new patients for this kind of treatment?”
The goal is to make sure the clinic has experience with this medication and that they are open to evaluating new patients.
Some clinics allow online booking. In these cases, it is helpful to send a secure message through the clinic’s portal to ask about tirzepatide before selecting an appointment time.
Sharing Insurance Information Early
When speaking with the clinic, it is useful to share insurance information upfront. Insurance coverage for tirzepatide can vary. Some insurance plans require prior approval or special paperwork before the medication can be prescribed.
The clinic may ask for the following:
- Insurance provider name
- Policy number
- Type of plan (such as HMO, PPO, Medicare, or Medicaid)
- Whether there is prescription drug coverage
Giving this information early can save time later. It helps the clinic staff check what is needed before the first visit and prepare any documents for prior authorization if needed.
Choosing the Right Appointment Type
Clinics may offer different types of appointments. It is important to book the right one. These are the most common options:
- Initial Consultation: This is a longer visit where the provider learns about the patient’s health history. This appointment is often required before starting tirzepatide.
- Injection Visit: If the medication has already been approved and prescribed, a separate appointment may be needed for teaching how to inject it or for receiving the first dose in the office.
- Follow-Up Visit: These are for patients who have already started tirzepatide and need to check in about results, side effects, or dose changes.
When booking, the clinic’s scheduler may ask the purpose of the visit. Saying something like “a consultation to discuss tirzepatide” or “to see if I qualify for Mounjaro® or Zepbound®” helps the staff assign the right provider and the right amount of time for the appointment.
Preparing for Scheduling Delays
Some clinics have long wait times for appointments, especially those that focus on weight management or endocrinology. It is helpful to ask about next available dates and if the clinic keeps a waitlist for earlier openings.
If the clinic cannot offer a timely appointment, they may suggest a referral to a different provider or a telehealth consultation if allowed in the state and under insurance guidelines.
Booking an appointment for tirzepatide treatment involves more than just picking a date and time. It requires asking the right questions, providing insurance information early, and understanding the steps involved before receiving the medication. Good communication with the clinic can help ensure that the process goes smoothly and that the visit is focused and productive.
How to Prepare for the First Visit or Tirzepatide® Injection
Getting ready for the first visit with a healthcare provider for a tirzepatide® injection is an important step in the treatment journey. Whether the appointment is for a consultation or the first dose, preparation helps the process go smoothly and safely. This section explains what to bring, what to ask, and what to expect during the visit.
Important Documents and Information to Bring
Before the visit, it is helpful to gather certain medical records and other important documents. This information allows the provider to make informed decisions about care and helps avoid delays in starting tirzepatide®.
Items to bring include:
- Health insurance card: The office may need to check what insurance covers and if any approvals are required.
- A list of current medications: Include the name, dose, and how often each medication is taken. This helps the provider make sure tirzepatide® is safe to use with other prescriptions.
- Medical history records: If available, bring recent lab results, blood pressure readings, or diabetes test reports (such as A1C levels).
- Weight and BMI history: Some insurance plans require documentation of weight over time. This includes past weights, body mass index (BMI), and any past attempts at weight loss.
- Previous treatments tried: If other medications have been used for diabetes or weight loss, include this information. Some plans need proof that other treatments were tried before approving tirzepatide®.
Having this information ready saves time and helps the provider meet insurance requirements more quickly.
Learning How to Inject Tirzepatide®
Tirzepatide® is designed for once-weekly self-injection using a prefilled pen. At the first visit, the healthcare provider may show how to use the pen, or give instructions to practice with a training device. In some cases, a nurse or medical assistant may give the first injection while explaining each step.
Training usually includes:
- How to handle and store the pen: Tirzepatide® pens must be kept in the refrigerator but can stay at room temperature for a limited time once in use.
- Where to inject: The preferred injection sites are areas with fatty tissue. These include the stomach (away from the belly button), upper thighs, or the back of the upper arms.
- Proper technique: The trainer will explain how to clean the area, hold the pen, insert the needle, and complete the injection. Most pens have an automatic mechanism and do not require seeing or handling a needle directly.
- Disposal: Used pens must be placed in a sharps container. The provider will explain how to safely dispose of used devices.
Hands-on practice builds confidence. If needed, patients can ask for a repeat demonstration or printed instructions to take home.
Time and Logistical Considerations
The first appointment may take longer than a typical visit. It usually includes medical evaluation, education about the medicine, and possibly the first injection. Some offices ask patients to arrive early or bring the medication if it has already been picked up at a pharmacy.
It is also important to ask about:
- Clinic hours and availability for future visits
- Whether appointments are in-person or can be done by telehealth after the first visit
- If the clinic assists with insurance paperwork or pharmacy communication
Planning ahead can make the experience less stressful and more productive.
Preparing for the first tirzepatide® visit involves gathering medical information, asking clear questions, and learning how to use the injectable pen safely. Bringing the right documents and understanding what to expect during the appointment can help ensure a smooth start to treatment. Providers are there to explain the process and support each step along the way.
Are There Telehealth Options for Tirzepatide Consultations?
Tirzepatide is a prescription injection used to manage type 2 diabetes and support weight loss. Some people may wonder if they can use telehealth to get a tirzepatide prescription or learn how to use it. Telehealth—also called virtual care or online doctor visits—is becoming more common. But not all parts of care for tirzepatide can be done online.
This section explains when telehealth can be used for tirzepatide, when in-person visits are needed, and what to ask before using telehealth services. It also shares tips on how to check if telehealth is covered by insurance.
When Telehealth Can Be Used for Tirzepatide
Telehealth works well for many parts of the process, such as:
- Initial Consultations: Some providers offer first appointments online. During this visit, a doctor or nurse practitioner can review a patient’s medical history, weight, and current medications. They may also ask about symptoms, goals, and past treatments. Based on this information, the provider may decide to prescribe tirzepatide.
- Ongoing Monitoring: After the first dose, providers may use telehealth to check on progress. They can ask about side effects, weight changes, and blood sugar levels. This is useful for people who live far from a clinic or who have a busy schedule.
- Education and Support: Some clinics use telehealth to teach how to give the injection. A nurse or educator may demonstrate how to use the pen over video. This includes showing where to inject, how to hold the pen, and how to store the medicine.
- Prescription Refills: If the treatment is going well, the provider may use a telehealth visit to approve the next prescription. This can save time and reduce the need for in-person trips.
When an In-Person Visit Is Needed
Some steps in the tirzepatide process still require an in-person visit:
- First Injection or Training: Many clinics prefer to give the first shot in the office. This helps make sure it is done safely. A provider can watch for allergic reactions or side effects. After this first dose, future shots are usually done at home.
- Physical Exam or Lab Tests: If a patient needs blood tests, weight checks, or a physical exam, they may need to visit a clinic. Some insurance companies also ask for lab results or a recent weight check before they approve coverage.
- Prior Authorization Requirements: Sometimes, a provider must send medical records to an insurance company. If the records are not recent or clear, the provider may ask for an in-person visit to collect the right information.
- Complications or Concerns: If a patient has severe side effects or if the medicine does not seem to be working, a face-to-face exam may be needed to find the problem.
State and Insurance Rules for Telehealth Prescriptions
Different states have different rules about telehealth and prescriptions. In some states, a doctor can prescribe a medicine like tirzepatide after a video call. In others, an in-person visit must happen first. Patients who move across state lines may need to see if the provider is licensed in both places.
Insurance coverage also varies. Some plans cover telehealth the same way as in-office visits. Others may only cover certain telehealth platforms or approved providers. Patients should check if their insurance plan:
- Covers video or phone visits for weight management or diabetes care
- Includes the provider or clinic offering the telehealth visit
- Allows prescriptions for injectable medications through telehealth
How to Find a Telehealth Provider for Tirzepatide
To find a provider that offers tirzepatide through telehealth, look for:
- Endocrinologists or obesity specialists who offer virtual care
- Weight loss clinics that provide GLP-1 or GIP/GLP-1 medications
- Online healthcare platforms that list medications like tirzepatide
It is important to make sure the provider is licensed and experienced with this type of treatment. Some programs may be out-of-pocket and not covered by insurance. Always ask about pricing, prescription rules, and how the medication will be shipped or picked up.
Examples of Brand Names
Tirzepatide is sold under the brand name Mounjaro®, made by Eli Lilly. Any telehealth provider offering tirzepatide must follow the rules for prescribing Mounjaro®. This includes checking for medical need and confirming that it is safe for the patient.
Telehealth makes care easier for many people, but it may not replace all in-person visits. Before starting virtual care, it is helpful to check with both the provider and the insurance plan to make sure everything is in place. With the right steps, telehealth can be a safe and convenient way to begin or continue tirzepatide treatment.
What Do I Need to Know About Follow-Up and Refill Appointments?
After starting tirzepatide treatment, follow-up and refill appointments are an important part of ongoing care. These visits help doctors monitor progress, adjust the dose when needed, and manage any side effects. They also ensure the medication is refilled on time and taken correctly. Staying on schedule helps tirzepatide work more effectively and safely.
Follow-Up Appointment Schedule
Doctors usually schedule regular follow-up appointments after a patient begins tirzepatide. These visits often happen every 2 to 4 weeks at the start of treatment. After the right dose is reached and there are no side effects, follow-up appointments may occur every 1 to 3 months.
These visits are used to:
- Check weight changes: Tirzepatide is used to manage type 2 diabetes and support weight loss. Doctors track weight loss over time to measure progress.
- Review blood sugar levels: For people with type 2 diabetes, blood sugar results may be reviewed through finger-stick logs or lab tests like A1C.
- Adjust the dose: Tirzepatide is usually started at a low dose and slowly increased. This helps reduce side effects like nausea or stomach pain. Follow-up visits are when doctors decide whether to raise the dose or keep it the same.
- Check for side effects: Some patients may have side effects from tirzepatide, such as upset stomach, vomiting, or fatigue. Follow-up appointments are a time to talk about these problems.
- Review injection technique: If the medication is self-injected at home, doctors may check that the injection is being done correctly.
Dose Titration and Monitoring
Tirzepatide, such as the brand name Mounjaro®, is started at a low dose. The dose is usually increased every 4 weeks until the right level is reached. The most common doses are 2.5 mg, 5 mg, 7.5 mg, 10 mg, 12.5 mg, and 15 mg once per week. Not everyone needs the highest dose. Doctors decide the best dose based on how well the medicine is working and if there are any side effects.
Each time the dose is changed, another follow-up appointment is often scheduled. This is important for checking how the body reacts to the new dose and making sure the patient is still doing well.
Refill and Prescription Management
Tirzepatide is a prescription medication and must be refilled regularly. Depending on the pharmacy and insurance, prescriptions are often written for 1 month at a time, with a set number of refills allowed.
Here are key points to understand about refills:
- Prescription refills may require follow-up visits: In some cases, the doctor may not allow unlimited refills. A new appointment may be required before another prescription is written.
- Pharmacies may have delays: Some pharmacies may need extra time to order tirzepatide, especially if it is in high demand or requires special handling. It is a good idea to request a refill several days before running out of medication.
- Specialty pharmacies may be used: Some patients get tirzepatide from specialty mail-order pharmacies. These pharmacies may need confirmation from the doctor before sending the next dose.
Managing Missed Appointments or Delayed Refills
Missing an appointment or running out of medication can delay treatment. If a dose is missed, it may affect how well tirzepatide works. If a scheduled follow-up is missed, it could delay dose changes or cause refill problems.
To help prevent issues:
- Keep a calendar or reminder for all appointments.
- Ask the clinic staff if an appointment is required before each refill.
- If a refill is delayed or denied by the pharmacy or insurance, contact the doctor’s office quickly.
Coordinating with the Clinic and Insurance
Some refills require approval from the insurance company. This is called “prior authorization.” If the dose has changed, or if the treatment is being renewed after a pause, the doctor may need to send new paperwork. Clinic staff often handle this process, but it can take several days.
It is also helpful to:
- Let the clinic know about any changes in insurance.
- Make sure the pharmacy and clinic have up-to-date contact information.
- Keep track of how many doses are left so there is time to manage any delays.
Ongoing care with tirzepatide includes routine follow-up visits and on-time prescription refills. These steps are necessary to monitor health, adjust the dose safely, and avoid interruptions in treatment. Good communication with healthcare providers and pharmacies helps make the process smoother and supports better health results.
Conclusion
Tirzepatide is a prescription medicine used to help manage type 2 diabetes and, in some cases, assist with weight loss under a doctor’s supervision. It is given as a shot under the skin, usually once a week. While the medicine itself has gained attention for its effects, getting access to a tirzepatide shot involves several important steps. Patients need to know how to find doctors or clinics that provide this treatment, how to deal with insurance coverage, and what to expect when making appointments or picking up prescriptions.
Doctors who can prescribe tirzepatide include primary care physicians, endocrinologists, and obesity medicine specialists. Nurse practitioners and physician assistants may also provide this treatment, depending on local regulations and clinic policies. Many patients start by speaking with their regular doctor. If the doctor does not prescribe tirzepatide, the patient may be referred to a specialist. Certain clinics may focus on diabetes or weight management and may be more familiar with this medication and how to use it properly.
Finding a clinic that offers tirzepatide can be done in several ways. Some people use online tools provided by healthcare systems or insurance companies to search for doctors. These directories often allow users to filter by specialty, location, and treatments offered. Some drug manufacturers also offer provider locator tools on their websites. A phone call to a nearby clinic or doctor’s office can help confirm whether they prescribe tirzepatide.
Pharmacies are also part of the process, but tirzepatide is not something that can be picked up and used right away like over-the-counter medicine. After getting a prescription, some patients may receive training at the clinic on how to give themselves the shot at home. In other cases, the injection is given at the clinic itself. Not all pharmacies carry tirzepatide, as it may be classified as a specialty drug. Sometimes, it is sent through the mail by a specialty pharmacy.
Insurance is a key part of accessing tirzepatide, especially since it can be expensive without coverage. Most patients need to check with their insurance provider to see if the drug is on the list of covered medications, called a formulary. Insurance plans often require a process called prior authorization. This means the doctor must provide medical records showing that tirzepatide is necessary. Some plans ask for proof of past treatments that did not work before they approve coverage for tirzepatide. Others may cover it only for people with certain medical conditions, such as a high body mass index (BMI) or type 2 diabetes.
Some of the common challenges with insurance include high co-pays, limited quantities approved per month, and denials based on missing information. To improve the chances of approval, doctors and clinic staff usually prepare detailed paperwork. This may include medical history, body measurements, and notes about other treatments. Patients often need to follow up with the insurance company or clinic to track the approval process. If coverage is denied, an appeal can sometimes lead to approval.
Once coverage is confirmed and the doctor has prescribed the medication, patients can book an appointment. The first appointment may involve a full check-up and questions about health history. Some clinics also use the time to teach the patient how to give the injection safely. Preparing for this visit may include bringing an insurance card, a list of current medications, and recent lab results if available.
In some situations, telehealth is an option. Doctors can meet with patients by phone or video to discuss the medication and decide whether to prescribe it. Some steps, like giving the first injection or teaching injection techniques, may still require an in-person visit. Each clinic or state may have its own rules about what can be done by telehealth and what must be done in person.
Follow-up appointments are an important part of care. These visits may include tracking weight, checking blood sugar, and adjusting the dose if needed. Refills may also be reviewed during follow-up visits. If the shot is self-administered, a new prescription must be sent to the pharmacy before the next dose runs out. Some pharmacies may offer automatic refill reminders or delivery options.
Overall, getting a tirzepatide shot is a step-by-step process. It starts with finding the right doctor, making sure insurance will cover the cost, and preparing for the first visit. Understanding each step can help avoid delays and make treatment smoother. Brand names like Mounjaro® may be used when prescribing tirzepatide, and it’s important to follow the instructions given by healthcare providers. With the right support, many patients are able to begin treatment successfully and continue with regular follow-up to manage their health.
Research Citations
U.S. National Library of Medicine. (n.d.). A study of tirzepatide at different injection sites in participants with different body sizes. ClinicalTrials.gov. Retrieved August 21, 2025, from ClinicalTrials.gov registry.
Eli Lilly and Company. (2024, December 19). Are there safety or efficacy differences between tirzepatide injections in the abdomen versus thigh versus upper arm? In Zepbound® (tirzepatide) injection – FAQ. Retrieved August 21, 2025.
Ro. (2025, June 15). Where and how to inject tirzepatide: Step-by-step guide. Retrieved August 21, 2025.
Trim Body M.D. (n.d.). Where and how to inject tirzepatide: Weight-loss guide. Retrieved August 21, 2025.
Allure Aesthetic. (2025, March 26). Best place to inject tirzepatide for weight loss. Retrieved August 21, 2025.
Seladi-Schulman, J. (2025, May 8). Mounjaro injection sites: Where and how to inject. Medical News Today. Retrieved August 21, 2025.
U.S. National Library of Medicine. (2025, January 15). Tirzepatide injection: MedlinePlus Drug Information. MedlinePlus. Retrieved August 21, 2025.
Mizumoto, J. (2023). Tirzepatide-induced injection-site reaction. Cureus. Article 188359.
Wikipedia contributors. (2025, August). Tirzepatide. In Wikipedia. Retrieved August 21, 2025.
The Sun – Fabulous. (2025, July 10). I can’t go to work & am scared to move from the loo because of Mounjaro… but people say it’s down to WHERE I’m injecting. The Sun. Retrieved August 21, 2025.
Questions and Answers: Tirzepatide Shot Locations
Tirzepatide is typically injected subcutaneously (under the skin) in the abdomen, thigh, or upper arm.
The abdomen is the most commonly used site, about two inches away from the navel.
No, you should rotate injection sites each time to avoid tissue damage or irritation.
All approved sites (abdomen, thigh, upper arm) provide effective absorption, so the choice is mostly personal comfort or convenience.
It should be injected into the fatty layer just beneath the skin (subcutaneous tissue), not into muscle.
Yes, the upper arm is a valid injection site, but it’s difficult to self-inject there, so someone else should administer it if you choose that location.
No, you should avoid injecting near scars, moles, stretch marks, or skin that is bruised, red, or irritated.
The buttocks are not an approved site for tirzepatide injections. Use only the abdomen, thigh, or upper arm.
Try to use a different area within your chosen injection site each week, spacing injections at least an inch apart.
Yes, always clean the injection site with an alcohol swab and let it dry before injecting to reduce the risk of infection.