Table of Contents
Introduction
Embarking on a weight loss journey is a pivotal decision that extends beyond physical transformation, influencing emotional and psychological well-being. When traditional methods fall short, Medical Weight Loss emerges as a scientifically-backed alternative. Here, healthcare professionals design, guide, and oversee weight loss strategies to ensure they are safe, effective, and sustainable, transforming your path to better health.
The global rise in obesity is now a critical public health crisis. The World Health Organization (WHO) highlights the serious consequences of excess weight, including cardiovascular diseases, diabetes, and certain cancers. Addressing this growing epidemic requires a focus on effective and safe weight loss strategies.
This article aims to clarify the concept of medical weight loss by outlining its key components, processes, benefits, and risks. We will explore its evidence-based methodology, demonstrating its relevance and effectiveness in a world increasingly burdened by weight-related health issues. Join us as we dive into real-life examples, scientific research, and expert opinions, offering a comprehensive understanding of this specialized approach to weight management that goes beyond just counting calories.
Medical weight loss has the potential to be a guiding light for those struggling with weight management, and it could play a crucial role in fostering a healthier, more balanced society.
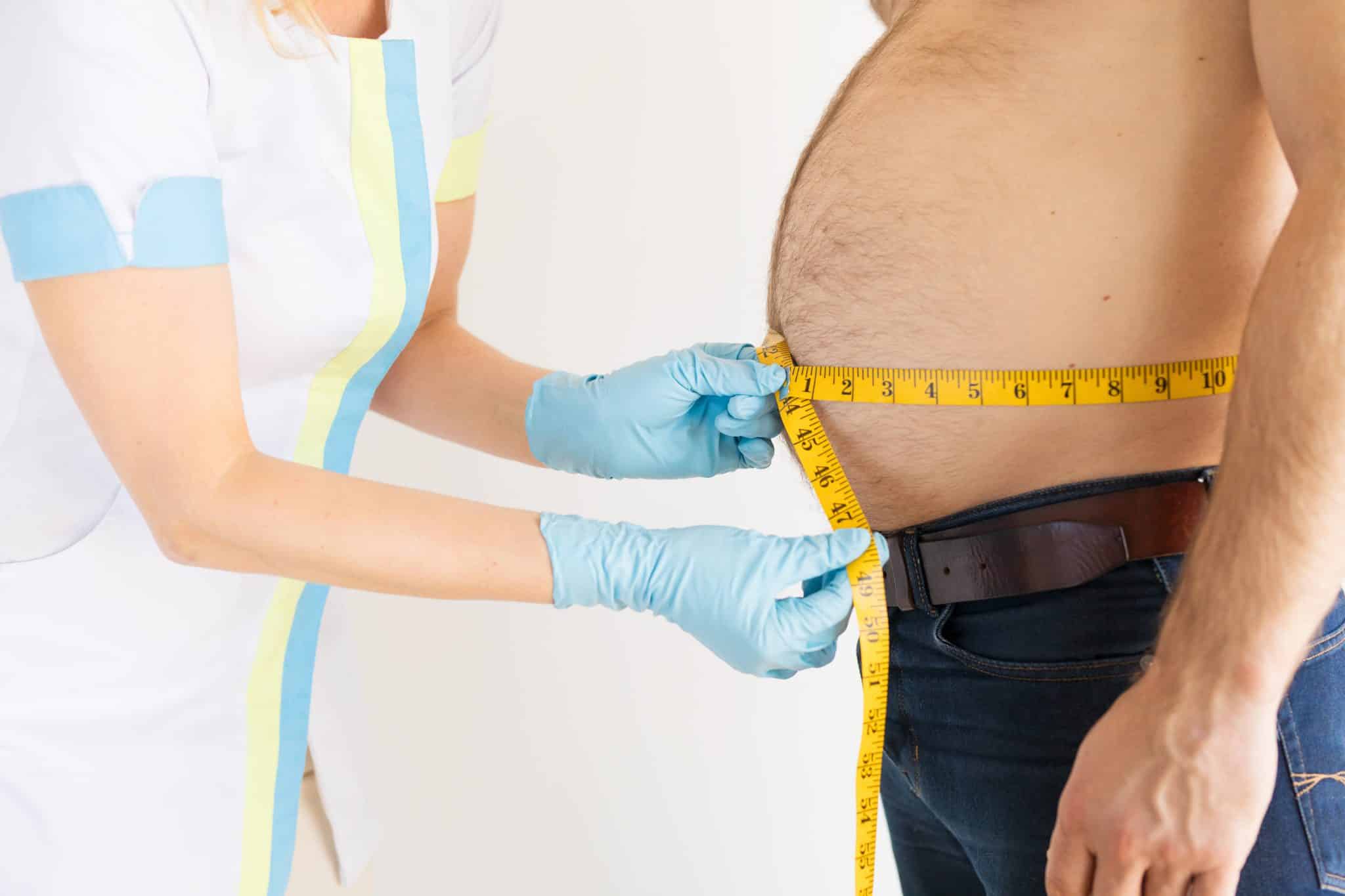
In a world where convenience often trumps nutrition, the obesity epidemic looms large, posing a significant threat to global health. According to the WHO, around 2.8 million people die annually due to being overweight or obese, highlighting a crisis with far-reaching consequences beyond appearance or societal norms. Obesity affects all demographics, cutting across age, gender, and socioeconomic status, demanding urgent and informed intervention.
The impact of obesity is profound, touching every aspect of life—biological, psychological, and social. Medically, obesity is a precursor to serious health conditions such as Type 2 diabetes, heart disease, stroke, and certain cancers. As Body Mass Index (BMI) increases, so do these risks. Mental health also suffers, as the struggle with weight, societal pressure, and repeated failures to lose weight can lead to depression, anxiety, and low self-esteem.
Economically, obesity is a heavy burden, increasing healthcare costs and reducing productivity. Lost workdays, decreased productivity, and early death take a significant toll on economies, diverting resources from other essential needs.
The factors driving this epidemic are complex, including the proliferation of high-calorie, low-nutrient foods, sedentary lifestyles enabled by technology, and even genetic predispositions. These elements often intertwine with psychological factors, where food becomes a means of emotional regulation, complicating efforts at sustainable weight management.
Understanding the profound impact and intricate nature of the obesity epidemic is crucial for developing targeted, effective interventions like medical weight loss. As we explore various weight loss methods, remember that the journey to a healthy weight is not just about reducing calories—it involves a holistic approach that considers the entire person: body, mind, and environment.

Traditional Weight Loss Methods
When starting a weight loss journey, many people turn to traditional methods, hoping for success. These approaches include a wide array of diets, exercise routines, and lifestyle changes, each claiming to be the key to effective weight management. However, the reality is often more complex, with many individuals finding these methods confusing, contradictory, and ultimately frustrating.
Dietary Approaches:
Dieting is often the first step in traditional weight loss. From low-carb diets like Keto to calorie-counting plans and plant-based options, the choices are endless. While some people achieve their goals with these diets, many others face constant trial and error, leading to frustration and temporary results. Nutritional imbalances are also a common risk, further complicating the process.
Exercise Regimens:
Exercise is another cornerstone of traditional weight loss. Activities range from cardio and strength training to yoga, each offering unique benefits. Yet, for those with significant weight to lose or underlying health conditions, these routines can be overwhelming, inaccessible, or even dangerous. This often necessitates alternative or supplementary strategies.
Challenges in Traditional Methods:
The concept of “calories in, calories out” seems simple, but in practice, traditional methods are fraught with challenges. Psychological barriers, metabolic adaptations, lifestyle constraints, and societal pressures often sabotage even the most determined efforts. As a result, many find themselves trapped in a cycle of weight loss and regain, known as “yo-yo dieting.”
The Need for Personalization:
A significant flaw in traditional methods is the lack of personalized support. The journey can feel isolating, lacking the comprehensive, multidimensional support needed to overcome physiological, psychological, and practical challenges. This gap often leads to repeated failures and discouragement.
In the following sections, we’ll introduce the concept of medical weight loss, which addresses these shortcomings by offering a more personalized, medically supervised, and structured approach. This method aims to create a weight loss journey that is not only effective but also sustainable and supportive in every aspect.
Understanding Medical Weight Loss
In the crowded arena of weight loss options, finding a solution that is both effective and sustainable leads us to the concept of medical weight loss. This approach goes beyond conventional methods by integrating scientific rigor with a personalized, multidisciplinary framework. Unlike generic weight loss strategies, medical weight loss is a comprehensive, medically supervised program that addresses the unique physiological, psychological, and social needs of each individual.
Medical weight loss is not just another diet or exercise plan; it is a tailored program designed to achieve sustainable results by focusing on overall health, rather than just numbers on a scale. This approach begins with a thorough medical evaluation, assessing an individual’s medical history, metabolic rate, and any underlying factors contributing to weight gain, such as hormonal imbalances or metabolic disorders. This evaluation informs a customized weight management plan that combines dietary, physical, and behavioral strategies, all under the continuous supervision and support of healthcare professionals.
Key to the success of medical weight loss is the use of FDA-approved weight loss medications, specialized dietary plans, exercise regimens, and when necessary, surgical interventions—all integrated with psychological support. This holistic approach ensures that weight loss is not a solitary struggle but a collaborative journey, adapting to the evolving needs and challenges of the patient.
What sets medical weight loss apart is its unwavering commitment to personalization, scientific methodology, and ongoing support. It transcends simple calorie counting, engaging with the individual to optimize health, vitality, and quality of life while achieving weight management goals. In the sections that follow, we will explore the essential components of medical weight loss, revealing how medical expertise, personalized planning, and a dedication to long-term health come together to guide individuals on their journey to sustainable well-being.
Core Components of Medical Weight Loss
Medical weight loss is a comprehensive approach designed to achieve sustainable weight management through a combination of critical components that work together to deliver real, lasting results.
Medical Supervision
Medical weight loss prioritizes your health and safety, with healthcare professionals like physicians and dietitians guiding you every step of the way. Their expertise ensures that your weight loss plan is not only effective but also tailored to minimize risks and enhance overall health. Continuous monitoring allows for the management of any pre-existing conditions, tracks your body’s response, and enables timely adjustments to keep your weight loss journey aligned with your evolving needs and goals.
Personalized Plan
The success of medical weight loss lies in its individualized approach. Every person has a unique combination of physiological, psychological, and social factors that influence weight management. Through thorough assessments and regular check-ins, healthcare providers create a customized plan that integrates diet, exercise, and behavioral strategies. This plan is specifically designed to match your health status, metabolism, lifestyle, and weight goals, ensuring a more effective and sustainable outcome.
Behavior Modification
Long-term weight management requires changes in deeply rooted habits, especially those related to diet and lifestyle. Medical weight loss programs incorporate behavior modification techniques to help you develop healthier habits and a mindset conducive to maintaining weight loss. Through education, psychological support, and strategic interventions, you gain the skills needed to overcome challenges, make informed decisions, and stay on track toward better health.
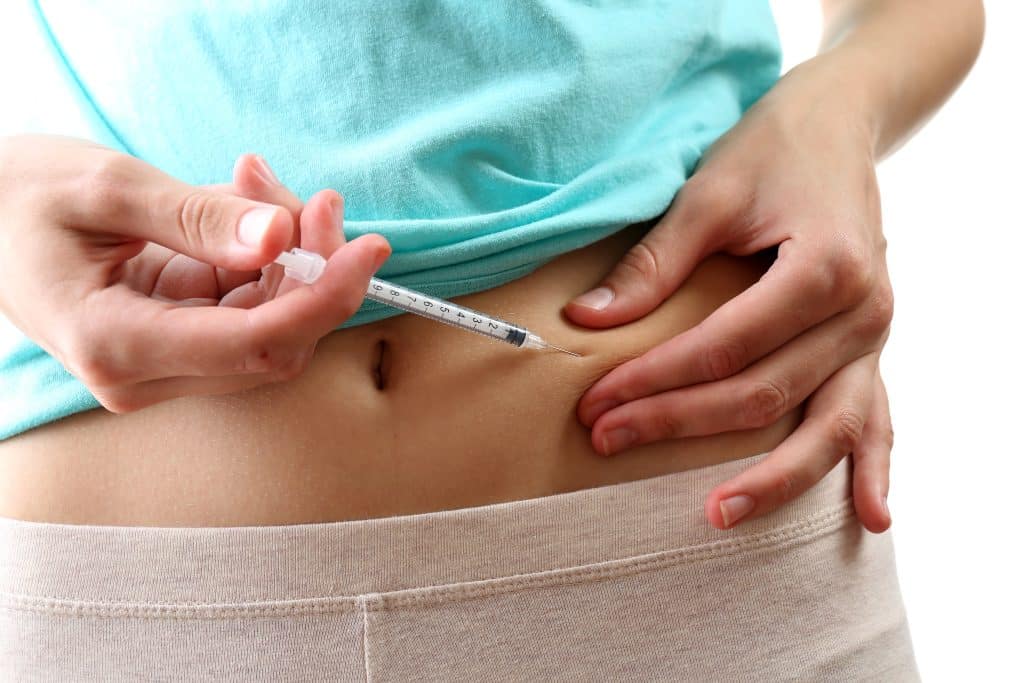
Medication
In some cases, FDA-approved weight loss medications may be recommended as part of your medical weight loss plan. These medications are carefully prescribed to complement dietary and exercise efforts, helping to curb appetite or address specific physiological challenges that hinder weight loss. Medication is always used as part of a broader, medically supervised strategy to ensure it is safe and appropriate for your situation.
Moving Forward
Medical weight loss is a science-backed approach that respects your individuality while striving for long-term health and well-being. In the next sections, we will dive deeper into the methodology, phases, and ongoing support that define this process, empowering you to not only reclaim your health but also transform your relationship with your body, food, and self.
Advantages and Challenges of Medical Weight Loss
In the complex journey toward effective and sustainable weight management, medical weight loss offers a structured, scientifically proven, and supportive approach. However, like any method, it presents both advantages and challenges that must be carefully considered.
Advantages
- Scientifically Proven Approach: Medical weight loss is grounded in evidence-based practices and medical guidelines, ensuring safe and effective strategies tailored to individual needs.
- Personalized Treatment: Each plan is customized to address the unique physiological, psychological, and lifestyle factors of the individual, making the approach highly specific and effective.
- Holistic Health Focus: Medical weight loss goes beyond shedding pounds; it targets overall health, addressing underlying medical conditions and improving overall well-being.
- Continuous Support: A dedicated multidisciplinary team provides ongoing support, offering guidance and adjustments as needed, ensuring a structured and adaptable plan.
- Behavioral Transformation: The integration of behavioral strategies helps rewire habits and mindsets, laying the foundation for long-term success.
Challenges
- Accessibility Issues: The cost of medical weight loss programs can be prohibitive, limiting access for many individuals.
- Time Demands: Success requires a significant time commitment, with regular consultations and adherence to the plan, which can be challenging for some.
- Over-Reliance on Medical Interventions: There is a risk of becoming overly dependent on medical interventions, which can undermine personal empowerment and self-management in the journey.
- Emotional Challenges: Delving into habits, emotions, and lifestyle changes can be emotionally taxing, often uncovering psychological issues that may require additional support.
- Managing Expectations: It’s crucial to set realistic expectations; medical weight loss is not a quick fix but a gradual, long-term approach that demands patience and perseverance.
Understanding the intricate balance of advantages and challenges in medical weight loss is key to crafting a successful, empathetic, and sustainable plan. By acknowledging and addressing the challenges, strategies can be developed to overcome them, while leveraging the advantages maximizes the potential for long-term success.
In the following sections, we will explore real-world applications, case studies, and delve deeper into how medical weight loss impacts not only physical health but also the personal journeys of those who undertake it, merging science with individual experiences of health and well-being.
Real-World Success Stories in Medical Weight Loss
Medical weight loss is not just a theoretical approach; it’s a transformative journey that has changed lives. By examining real-world examples, we can see the true impact of this science-backed method.
A Holistic Transformation
Consider an individual with chronic weight issues and newly diagnosed type 2 diabetes. Their medical weight loss journey began with a comprehensive evaluation of health, diet, physical activity, and psychological relationships with food.
A personalized plan was crafted by a team of experts, targeting both weight loss and blood sugar control. The diet was tailored to manage both weight and diabetes, while a customized exercise regimen was designed to match fitness levels and preferences.
However, the most crucial element of success was behavioral counseling. This component helped uncover and address emotional connections to food, gradually guiding the individual toward healthier, more sustainable habits. With continuous monitoring, the plan was adjusted as needed to ensure progress and maintain motivation.
Overcoming Setbacks
Another case highlights the challenges many face in weight management. After years of yo-yo dieting, this individual found themselves trapped in a cycle of weight loss followed by rapid regain. The emotional and physical toll was immense.
Medical weight loss offered a way out. The plan went beyond diet and exercise; it included a strong psychological support system that reshaped the relationship with food, body, and self. This support helped navigate setbacks, build resilience, and ultimately break free from the cycle that had held them back for so long.
The Power of Personalized Medical Weight Loss
These stories illustrate how medical weight loss can lead to profound transformations—physically, emotionally, and psychologically. Each journey is unique, but the potential for positive change is universal.
In the following sections, we will explore future advancements in medical weight loss, examining how innovations in science, technology, and psychology could further refine and enhance this comprehensive approach to health and well-being.
Future Directions in Medical Weight Loss
The future of medical weight loss is evolving rapidly, with new possibilities emerging from the intersection of technology, medical science, and psychology. Here’s a look at the key areas shaping this transformation:
Technological Innovations
Technology is revolutionizing medical weight loss. Wearable devices and health apps are no longer just tracking steps—they’re monitoring vital signs, diet, and mental health. Artificial Intelligence (AI) is at the forefront, enabling personalized plans that adapt in real-time, optimizing strategies for lasting results.
Advancements in Medical Science
Ongoing research is expanding our understanding of metabolism, nutrition, and genetics, leading to breakthroughs in weight loss. For example, insights into the microbiome are paving the way for treatments that optimize gut health to support weight management. Research on hormones like leptin and ghrelin is also opening doors to more targeted and effective medications.
Psychological Approaches
Recognizing the strong connection between mental and physical health, future weight loss strategies will integrate psychological support more deeply. Techniques like Cognitive-Behavioral Therapy (CBT), mindfulness, and even virtual reality can help foster a mindset that supports long-term healthy habits.
Personalized Medicine
Personalized medicine is set to revolutionize weight loss by tailoring strategies to individual genetic and metabolic profiles. This could lead to customized diets that maximize nutrient absorption and minimize deficiencies, ensuring a more effective and sustainable approach to weight management.
Inclusivity and Accessibility
The shift towards holistic and inclusive healthcare means future weight loss programs will be more accessible and culturally sensitive. These programs will aim to be affordable and available to all, democratizing health and wellness.
The future of medical weight loss is bright, promising methods that are more effective, personalized, and inclusive. As we continue to embrace technological, scientific, and psychological advancements, we move towards a future where weight management is holistic, sustainable, and empathetically aligned with the diverse needs of individuals.
Conclusion
In the evolving field of medical weight loss, we are shaping a future that blends scientific precision with personalized care, all while deeply considering the complex human experience. This approach integrates the physical, psychological, and social aspects of health, transforming weight management into a comprehensive journey toward overall well-being.
Medical weight loss is grounded in scientific principles, driven by personalized and medically supervised strategies, and aims for long-term health. This multidisciplinary approach, combining medical oversight, tailored plans, behavioral change, and, when needed, medication, offers a clear and supportive path to better health.
Looking ahead, we anticipate a future where advancements in technology, deeper medical insights, and a better understanding of psychological factors will make medical weight loss even more effective, accessible, and compassionate. Continued research and innovation are key to ensuring that this approach remains empathetic and responsive to the diverse needs of individuals.
Medical weight loss is not just a method; it’s a transformative journey that acknowledges the complex nature of health. It offers a chance to redefine how we think about weight management, creating an environment where everyone feels supported, respected, and empowered on their path to better health. Take the first step toward a healthier future with medical weight loss today!
Research Citations
Medical weight loss refers to supervised weight management programs provided by healthcare professionals, typically involving a combination of dietary modifications, physical activity recommendations, behavioral therapy, and sometimes pharmacotherapy or surgical interventions for individuals with obesity or overweight. Here are some research citations that discuss medical weight loss programs:
- Kushner RF, Ryan DH. Assessment and lifestyle management of patients with obesity: clinical recommendations from systematic reviews. JAMA. 2014;312(9):943-952. doi:10.1001/jama.2014.10432
- Wadden TA, Webb VL, Moran CH, Bailer BA. Lifestyle modification for obesity: new developments in diet, physical activity, and behavior therapy. Circulation. 2012;125(9):1157-1170. doi:10.1161/CIRCULATIONAHA.111.039453
- Colquitt JL, Pickett K, Loveman E, Frampton GK. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;(8):CD003641. doi:10.1002/14651858.CD003641.pub4
- Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. J Am Coll Cardiol. 2014;63(25 Pt B):2985-3023. doi:10.1016/j.jacc.2013.11.004
- Apovian CM, Aronne LJ, Bessesen DH, et al. Pharmacological management of obesity: an endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2015;100(2):342-362. doi:10.1210/jc.2014-3415
- Kushner RF, Sorensen KW. Lifestyle medicine: the future of chronic disease management. Curr Opin Endocrinol Diabetes Obes. 2013;20(5):389-395. doi:10.1097/MED.0b013e328364d2eb
- Ryan DH, Johnson WD, Myers VH, et al. Nonsurgical weight loss for extreme obesity in primary care settings: results of the Louisiana Obese Subjects Study. Arch Intern Med. 2010;170(2):146-154. doi:10.1001/archinternmed.2009.489
- Anderson JW, Konz EC, Frederich RC, Wood CL. Long-term weight-loss maintenance: a meta-analysis of US studies. Am J Clin Nutr. 2001;74(5):579-584. doi:10.1093/ajcn/74.5.579
- Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. J Am Coll Cardiol. 2014;63(25 Pt B):2985-3023. doi:10.1016/j.jacc.2013.11.004
- Wadden TA, Butryn ML, Wilson C. Lifestyle modification for the management of obesity. Gastroenterology. 2007;132(6):2226-2238. doi:10.1053/j.gastro.2007.03.051
These studies provide insights into the various components and approaches to medical weight loss, emphasizing the importance of comprehensive, evidence-based interventions for effective long-term weight management.
Questions and Answers: Medical Weight Loss
Medical weight loss is a medically supervised approach to weight management. It involves healthcare professionals creating personalized weight loss plans based on an individual’s medical history, physical condition, and weight loss goals. These plans often include diet and exercise recommendations, behavioral therapy, and sometimes prescription medications or other medical interventions.
Unlike self-guided diet and exercise programs, medical weight loss is a comprehensive, structured approach overseen by healthcare professionals. It offers a personalized plan that may include medical diagnostics, tailored dietary strategies, prescribed physical activities, behavioral counseling, and, when appropriate, prescription medications. This method considers the patient’s overall health, addressing any underlying medical conditions and ensuring a safe and effective weight loss journey.
Medical weight loss is generally considered safe as it is conducted under the supervision of healthcare professionals. This supervision ensures that the weight loss plan is not only effective but also tailored to the patient’s health needs, reducing the risks associated with unsupervised weight loss methods.
Individuals who have struggled with weight loss, those who are overweight or obese, and people with weight-related health issues like diabetes or heart disease can benefit from medical weight loss. It is also suitable for those seeking a structured and supervised approach to weight management.
The duration of a medical weight loss program varies depending on individual goals, starting weight, and specific health needs. Programs can range from a few months to a year or more for ongoing weight management.
A typical medical weight loss program includes an initial medical assessment, a personalized weight loss plan, regular follow-up appointments for monitoring progress, dietary and exercise guidance, behavioral counseling, and, if necessary, prescription medications or other medical treatments.
Yes, medical weight loss can be particularly beneficial for individuals with conditions like diabetes or high blood pressure. Weight loss often leads to improved management of these conditions, and the supervised nature of the program ensures that any dietary and exercise plans are safe and effective for patients with specific health concerns.
No, prescription medications are not always used in medical weight loss programs. They are prescribed based on the individual’s health needs and medical history. The primary focus is usually on lifestyle changes such as diet and exercise.
Medical weight loss programs typically involve a team of healthcare professionals, including doctors, dietitians, exercise physiologists, and sometimes psychologists or behavioral therapists.
The cost of medical weight loss programs varies widely and depends on the specific services included. Some aspects of the program, such as medical consultations and certain medications, may be covered by insurance, but coverage varies. It’s advisable to check with insurance providers and medical facilities for specific cost information.

Dr. Jay Flottman
Dr. Jay Flottmann is a physician in Panama City, FL. He received his medical degree from University of Texas Medical Branch and has been in practice 21 years. He is experienced in military medicine, an FAA medical examiner, human performance expert, and fighter pilot.
Professionally, I am a medical doctor (M.D. from the University of Texas Medical Branch at Galveston), a fighter pilot (United States Air Force trained – F-15C/F-22/AT-38C), and entrepreneur.